The owners of an aging northwest Georgia hospital want to replace it with a smaller state-of-the-art facility about 5 miles away and closer to I-75. Under the state’s regulatory certificate-of-need (CON) system, other hospitals can contest CHI Memorial Hospital Georgia’s bid to get state approval for the replacement hospital, which would be located in Ringgold….
Tag: Hospitals
Fulton chairman floats tax hike as East Point hospital exit looms
By Ariel Hart and Andy Miller Facing the looming closure of a hospital in East Point, Fulton County officials and Grady Health System representatives are discussing ways to continue providing for emergency and hospitalization needs in the underserved south county area. Among the options: Raising the amount of money Fulton County taxpayers provide to the…
Wellstar closing ER, hospital beds at struggling East Point site, still seeks partner
Wellstar Health System in recent years has been exploring options – including a sale or partnership — for its Atlanta Medical Center and an affiliate hospital in East Point. A different option unfolded Wednesday: Wellstar announced that it’s converting the 200-bed East Point hospital into a primary care, outpatient and rehabilitation center. The ER and…
State hits Anthem with whopping fine for insurance violations
By Rebecca Grapevine and Andy Miller The state insurance department has levied a $5 million fine against health insurer Anthem Blue Cross Blue Shield, the largest such penalty in the agency’s history, for violations of state law involving medical providers and consumers. Insurance Commissioner John King, at a Tuesday news conference at the State Capitol,…
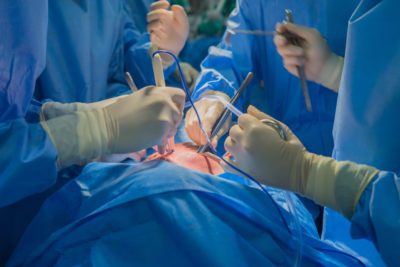
Bill in Legislature targets dangerous ‘surgical smoke’
In operating rooms, the smoke created by surgery can be a health hazard for those breathing it in. Such “surgical smoke’’ is a byproduct of the thermal destruction of human tissue by the use of lasers or other devices. According to the CDC, the smoke has been shown to contain toxic gases, vapors and particulates,…
Latest bill to overhaul health care regulations appears doomed
A sweeping bill to repeal the state’s health care regulatory process failed to clear the House by a crucial legislative deadline Tuesday, meaning it is probably dead for the year. The regulatory system, known as certificate of need (CON), governs much of how the health care industry operates in Georgia. A medical provider must apply…
CON opponents win a round in latest legislative fight over health care regulations
It wouldn’t be a Georgia General Assembly session without a fierce debate about the state’s health care regulatory apparatus. That system, known as certificate of need (CON), mostly governs how the health care industry functions in the state. It has been targeted annually by legislators proposing reforms to relax its rules. But these bills have…
The Piedmont powerhouse: Health system’s expansion reaches Augusta
Piedmont Healthcare has added Augusta to its expanding hospital footprint. The Atlanta-based nonprofit system now contains 19 hospitals, with the announcement Tuesday that it has taken over University Health Care System, which includes University Hospital in Augusta. Other hospitals in the agreement are smaller facilities: University Hospital Summerville and University Hospital McDuffie. The two systems…
Health care day: Bills on HIV, pregnancy, vaping, lead, caregivers move on
The Georgia House passed legislation Tuesday that could give Medicaid coverage to thousands of uninsured residents who have HIV. The chamber approved House Bill 1192 with a bipartisan 136-14 vote. If enacted by the General Assembly, the legislation would instruct the state’s Department of Community Health to apply to the feds for a waiver that…
More penalized Georgia hospitals . . . and more controversy
By Jordan Rau and Andy Miller Medicare has penalized 21 Georgia hospitals for having the highest rates of patient infections and potentially avoidable complications. That’s up slightly from the 18 hospitals in the state that drew penalties in the last round of federal assessments. For the penalized hospitals, Medicare payments are reduced by 1% for…