Part 5 of a Special Report The concept isn’t exactly new. Free-standing ERs — affiliated with hospitals but not physically connected to them — have cropped up in many areas, generally in suburban or urban locations where large numbers of local residents have private insurance. They provide emergency medical services apart from a regular hospital…
Tag: Rural Health
The ripple effect when rural hospitals drop birthing services
This is Part 3 of a Special Report Madelaine Austin is having her first baby, and had planned to give birth at Stephens County Hospital in northeast Georgia, just five minutes from her home. But in the middle of her pregnancy, she was forced to change OB/GYNs and the facility where she would deliver her…
How rural health care ‘limps along’ in certain communities
This is Part 2 of a Special Report The medical predicament that many rural communities want to avoid lies 35 miles south of Columbus, Georgia. Eight years ago, Stewart Webster Hospital, in a financial tailspin, closed its doors for the last time. Now weeds and trash litter the grounds around the facility. In the years…
A rural Georgia community reels after hospital closes
Lacandie Gipson struggled to breathe. The 33-year-old woman with multiple health conditions was in respiratory distress and awaiting an ambulance. About 20 minutes after the emergency call, it arrived. The Cuthbert home where Gipson lived was less than a mile from Southwest Georgia Regional Medical Center, but the ambulance couldn’t take her to the one-story…
Georgia to get less monoclonal antibodies as feds take over supply
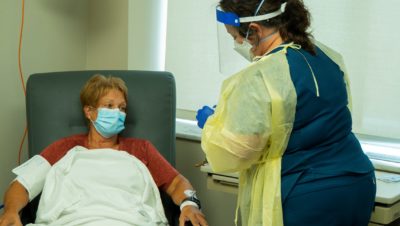
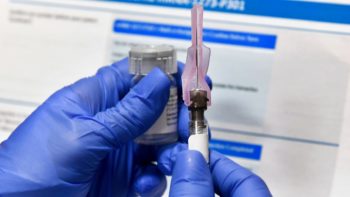
A recent surge in demand for powerful Covid antibody drugs has generated concerns about supply shortages in states that are heavy users of the treatment, including Georgia. About 70 percent of these lab-created drugs are being used in the Southeast. With that uneven distribution, federal health officials recently decided to take over supplies and allocate…
Covid surge eases slightly, but swamped hospitals see no relief
The state’s Covid cases and hospitalizations have dipped over the past week, Georgia health officials have reported. But that drop isn’t relieving the pressure on the front lines of hospitals — both smaller facilities and large urban centers. Take Appling Healthcare, which operates a rural hospital of 34 beds in Baxley, in southeast Georgia. The…
Rural Georgia counties reeling from virus onslaught
“It feels like it just doesn’t end.’’ That’s how Damien Scott, CEO of Emanuel Medical Center in rural southeast Georgia, described the current covid wave and its impact on his hospital and community. All six ICU beds at the Swainsboro hospital Tuesday morning were filled with very sick virus patients, with five on ventilators. Several…
As low vaccination rate fuels surge, Georgia hospital workers feel frustration, fatigue
The current covid onslaught may be the worst of the four virus surges in one crucial way: The effect on hospital employee morale. Leaders of Georgia hospital systems say the latest covid-19 wave has been very difficult for nurses and other clinical staff partly because it emerged at a time of wide availability of vaccines…
Hospital closure: A rural Black community loses a lifeline
This article first appeared in STAT, which gave Georgia Health News permission to republish it. Photos are by Bethany Mollenkof for STAT. By Olivia Goldhill In every corner of Latasha Taylor’s home are plants she knows nothing about. After years spent shirking her mother’s calls to join her in the yard at sunrise, Taylor now…
Black, Latino Georgians lag behind whites in COVID shots, report says
Blacks and Latinos in Georgia have significantly lower COVID-19 vaccination rates than whites, a newly released Kaiser Health News analysis shows. Thirty percent of whites in Georgia have had at least one shot, yet they trail another group — Asians, who are at 44 percent. The data were provided to KHN by the CDC in…