Georgia recorded its third straight day of high numbers of COVID deaths, with the 142 reported Thursday bringing the state’s three-day total to 424.
The new figure neared Tuesday’s record number of 145.
The medical strain from the post-holiday COVID surge, meanwhile, is being felt in hospitals across the state. And that pressure may increase even more, at least in the short term, experts say.
The state’s Department of Public Health reported more than 9,000 new COVID-19 infections Thursday. Georgia’s rate of positives on COVID tests is about 20 percent, far above the target level of 5 percent or less.

Grady Memorial Hospital, Atlanta’s safety-net giant, is at capacity.
The 162 COVID patients at Grady represent its highest total since the pandemic began, said Dr. Robert Jansen, Grady Health System’s chief medical officer. “It goes up every day,’’ he told GHN on Thursday.
Jansen said he doesn’t think the virus surge has yet peaked. “I think the crest of the surge will probably be in another seven to 10 days.’’
The state has reopened a 60-bed temporary hospital at the Georgia World Congress Center, a convention facility in downtown Atlanta. Jansen said there were 41 COVID patients there Thursday morning. “They’re coming from all over the state,’’ he said.
The patients at the center don’t require critical care services, Jansen added. Accommodating them there, however, relieves some of the pressure on hospitals treating sicker patients.
He said other large hospital systems in metro Atlanta, such as Wellstar, Emory, Piedmont and Northside, “are pretty much in the same shape we’re in. Everybody’s resources are stretched right now.”
The COVID vaccine, despite its rocky rollout, eventually will help curb the spread of the disease, he said, though “it’s too early now’’ to see that happening.
Pushed to the limit
Rising numbers of COVID hospitalizations are being reported across the state.
Wellstar Health System said Thursday that all 11 of its hospitals are seeing a surge in patient volumes, with most operating at full or over capacity. “We continue to monitor closely to ensure that we have the supplies, beds, and caregivers where they need to be,” Wellstar said in a statement. “Our greatest challenge currently is having enough staff to care for patients, many of whom are critically ill.”
The Marietta-based system said it has 730 COVID patients admitted to its hospitals, and another 81 under investigation for the disease.
Emory Healthcare also is seeing a big increase in hospitalized patients with COVID-19.
“We have surpassed the number of hospitalized patients with COVID-19 in critical and acute care as compared to any time since the pandemic started,” Emory said in a statement. “The rapid and continued rise in cases remains very concerning. Given the impact of holiday gatherings, we do not anticipate any reduction in cases over the next few weeks, which will only make a very difficult situation more extreme. We continuously monitor the capacity of our hospitals across Emory Healthcare to ensure we can care for all patients, with or without COVID-19.”
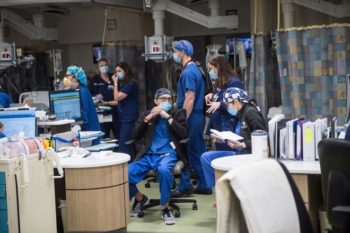
The Atlanta-based Northside Hospital System said it has seen a 365% increase in total COVID-19 patients over the last two months. COVID patients currently comprise 48% of Northside’s overall patient population.
In Augusta, hospitals are setting records when it comes COVID patients and then breaking those records a day or two later, the Augusta Chronicle reported Thursday.
“We’re doing a lot of very creative things to create capacity within the system,” said Dr. Phillip Coule, the chief medical officer at AU Health System, which set a record Thursday by treating 122 COVID-19 patients. “We’re currently over capacity right now, and that’s not including the patients that we are managing in other facilities via telemedicine.”
“We’re at capacity,” said Dr. John Farr, the chief medical officer for Doctors Hospital of Augusta, where there are 83 COVID-19 patients, two short of an all-time high. “It’s just that the patients don’t stop coming, so you have to find ways to create a little bit more capacity to take care of them. So capacity is a moving target.”
“If we need to convert additional areas, we’ll do what we need to do,” said Reyne Gallup, the executive vice president and chief operating officer for acute care services at University Hospital, which hit its high of 140 last week but has hovered just below that on most days since, the Chronicle reported.
Governor thanks, praises health workers
Gov. Brian Kemp, in his annual State of the State address on Thursday, praised health care workers for their heroism and sacrifice in fighting COVID-19.
Referring to the pandemic, Kemp said that “we can now see the light at the end of this tunnel,” and pointed out that 283,000 Georgians had been vaccinated as of Wednesday.

He said health care workers in Georgia have “literally faced hell on earth” during the 10 months of COVID-19. He specifically praised the work at Phoebe Putney Health System in Albany early in the pandemic. During that time, the Albany area, in southwest Georgia, had some of the worst COVID rates in the nation.
The pressure on health care workers is a big concern for Grady’s Jansen, who noted that the pandemic has unfolded amid a general nursing shortage. “We’re asking people to work longer and harder,’’ he said.
“The staff is stretched as thin as it can be,’’ Jansen said. “Nursing, housekeeping – everybody is working as hard as they can.’’

