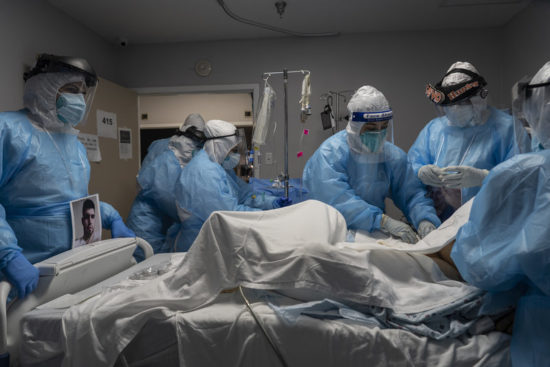
With Georgia topping 5,000 current hospitalizations for COVID-19, public health experts are calling for more state restrictions to curb the virus surge.
Yet another ominous factor popped up Tuesday: Georgia Public Health officials reported the state’s first case of the more contagious COVID-19 variant discovered in Britain last month and subsequently detected in several nations and U.S. states.
The variant was discovered during analysis of a specimen sent by a Georgia pharmacy to a commercial lab, state officials said. The Georgia resident is an 18-year-old male with no travel history, and is currently in isolation at home. Public Health said it’s working to identify close contacts of the individual and will monitor them closely and test them for the variant.
“So far, there is no evidence that the B.1.1.7 variant causes more severe illness or increased risk of death,’’ the state’s Department of Public Health said in a statement.
“The emergence of this variant in our state should be a wake-up call for all Georgians,” said the Public Health commissioner, Dr. Kathleen Toomey. “Even as we begin roll out of a COVID-19 vaccine, we must not let down our guard and ignore basic prevention measures – wear a mask, social distance and wash your hands frequently.”
In Britain, the fast-spreading variant led Prime Minister Boris Johnson to impose a strict new national lockdown, as the surge threatened to overwhelm the nation’s beleaguered hospitals, the New York Times reported.
After several days of frighteningly high and escalating case numbers, Johnson ordered schools and colleges in England to close their doors and shift to remote learning. The prime minister, who last year spent several days in the hospital with COVID-19, is appealing to people to avoid leaving home except for a few necessary activities, including essential work and buying food and medicine.
Hospital beds filling up
Aside from the variant threat, the hospital crisis in Georgia continues to escalate. On Monday, 90 percent of the hospital ICUs were filled.
The 5,124 COVID hospitalizations Monday in Georgia was a sharp rise from the 4,000 mark just eight days before. “Before that it took 10 days to go from 3,000 to 4,000,’’ said Amber Schmidtke, a microbiologist who publishes the Daily Digest, which tracks COVID in the state. Virus patients represent 31.2 percent of all hospitalized patients – an alarming percentage.

And a map from Brown University, which includes positives from antigen tests, shows that 158 of Georgia’s 159 counties “have disease rates that are beyond the point that contact tracing can isolate and manage cases,’’ Schmidtke said Monday. She noted that Liberty County in east Georgia was the only exception.
“Georgia is on fire with COVID-19,’’ she added.
“The demand this disease is placing on our health care system is intense.’’
Schmidtke urged a stronger state intervention, “whether that’s a mask mandate, a ban on gatherings, limiting indoor dining and bars and prioritizing outdoor service, etc. None of these things will be popular, but they also wouldn’t be forever. If asking people to do the right thing were a viable strategy, it would have worked by now. It hasn’t, so we need to do something else.’’
Gov. Brian Kemp previously issued a statewide stay-at-home order in April, along with other restrictions on businesses, but later lifted those rules.
A press spokesperson for Kemp could not be reached for comment on the potential for stronger restrictions.
A top infectious disease expert, Dr. Carlos del Rio of Emory University, told GHN on Tuesday that he was ‘’very, very concerned’’ about the capacity of the health care system to handle the increasing patient load from COVID.

“It is really bad right now and it’s going to get worse,’’ del Rio said.
If conditions deteriorate further, he said, doctors may have to tell patients who are sick that “there may not be a hospital bed for you.’’
“We’ve got to do something.’’ He said the COVID vaccinations — proceeding at a slow and uneven rate — “may not have a benefit for several weeks.’’
Del Rio suggested restricting social gatherings to 10 people or less (it’s now 50), and closing or limiting the operations of bars and restaurants.
More ‘hot spots’
Georgia communities are creeping up in the New York Times lists for COVID hot spots.
The Times, on its hot spot lists Tuesday, rated Dublin in Middle Georgia at No. 10 among U.S. metro areas in terms of new cases per capita over the past two weeks. And Upson County, also in Middle Georgia, was No. 15 Tuesday among county hot spots in the nation.
Public Health reported more than 10,000 new COVID cases Tuesday (including positives from rapid antigen tests).
Hospitals in other areas of the state are seeing the effect of the steady, huge numbers. About 40 Georgia hospitals reported Tuesday that they were on total ambulance diversion and/or on ICU/Critical Care diversion.
“The rest are extremely busy, and struggling with it,’’ said Jimmy Lewis, CEO of HomeTown Health, an association of rural hospitals in the state. “We’re trying to give care to patients in hospitals and give out vaccinations and placate the community at the same time.”
Tift Regional Medical Center in South Georgia said Monday that “we are still seeing a significant number of COVID-19 patients in the ER, which can contribute to longer than normal waits. Additionally, [the hospital] is still on critical care diversion. This means that our Intensive Care Unit is currently full and we have to refer patients to other hospitals which have open ICU beds.
In southwest Georgia, Phoebe Putney Health System reported Tuesday “a dangerous COVID-19 surge, and our latest projections indicate we are at least several weeks away from the peak of that surge.’’
In the past month, more than 30 of Phoebe Putney’s COVID-19 patients have died, said CEO Scott Steiner. “We are taking extraordinary measures to expand our capacity to handle the surge, including hiring additional staff and reorganizing staffing resources to maximize our COVID-19 clinical care capabilities.’’
And Gainesville-based Northeast Georgia Health System was treating 307 COVID-19 patients as of Tuesday, 14 more than the day before. There are no available beds in the ICU at Northeast Georgia Medical Center in Gainesville or the health system’s Braselton hospital. The system’s numbers set several records in recent weeks, the Gainesville Times reported.
Dr. Mark Ebell, a professor of epidemiology at University of Georgia’s College of Public Health, says such numbers show the need for strong action.
“We should have had a mandate for masks in public indoor spaces months ago,’’ Ebell said. “It’s unconscionable that we are one of the few states not to do so. We are now entering a critical time with cases increasing in Georgia due to holiday and New Year’s gatherings, and it is coinciding with when we also expect to see rising cases of influenza and pneumonia caused by other pathogens.’’
Ebell added that capping gatherings at 50 people “is way too high. It should be 10 as it is in many other states. There is just too high a chance that someone in a group of 50 is infected.
“I also think we have to decide what is more important to keep open for the next few months until vaccination is widespread: bars or schools?’’