One in four Georgia hospitals will be paid less by Medicare due to high rates of infections and patient injuries.
The 27 percent figure of eligible Georgia hospitals facing penalties is slightly above the national average, which is 25 percent.
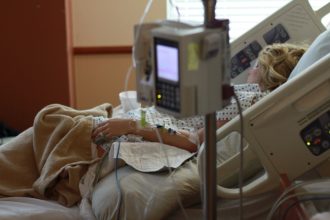
The Georgia hospitals facing pay reductions include some of the largest and best known. They include Grady Memorial Hospital in Atlanta; AU Medical Center in Augusta; Memorial Health University Medical Center in Savannah; Emory University Hospital and Emory University Hospital Midtown in Atlanta; Piedmont Columbus Regional Midtown and St. Francis Hospital in Columbus; and Coliseum Northside Hospital in Macon.
The percentage of Georgia hospitals being penalized for patient safety is significantly lower than last year’s figure, which was 35 percent. (Here’s a link to the Georgia hospitals facing penalties. Scroll down and plug “Georgia’’ into the All States search bar.)

In all, 800 hospitals in the United States will be paid less by Medicare this year because of high rates of infections and patient injuries, Kaiser Health News reported, citing federal records.
The number is the highest since five years ago, when the federal government launched the Hospital Acquired Conditions (HAC) Reduction Program, created by the Affordable Care Act, Kaiser Health News reported.
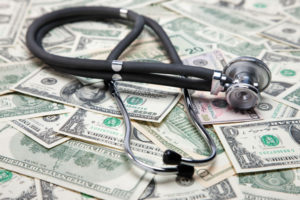
Under these penalties, each hospital will lose 1 percent of its Medicare payments for patients discharged between last October and this September.
The ACA created other penalties, such as annual payment reductions for hospitals with too many patients being readmitted within 30 days of discharge.
The safety penalties hit the hospitals that have the highest rates of infections, blood clots, cases of sepsis, bedsores, hip fractures and other complications. Each year, the quarter of general hospitals with the highest rates are punished, even if they have improved their record from the previous year.
Not all hospitals are included in the penalty program. Those exempted include small “critical access’’ hospitals and children’s hospitals.
The hospital industry has protested the HAC penalties, saying the program’s design creates an arbitrary cutoff for which institutions get punished and which don’t, KHN reported. The American Hospital Association said only about 41 percent of the 768 hospitals penalized in 2017 had HAC scores that were significantly higher than hospitals not being penalized.
“There are not statistical differences that would warrant a quarter of the hospitals in America getting a penalty,” said Nancy Foster, the association’s vice president for quality and patient safety.
Hospitals also complain that the statistics can be misleading. They say the facilities that do the best job testing for infections and other threats to patients can therefore appear to have worse problems, while their peers that are less diligent in identifying problems can appear better than they really are, KHN reported.
Separately, the CDC reported Tuesday that nearly 120,000 people contracted bloodstream staph infections in the United States in 2017, most of them in health care facilities – and nearly 20,000 died.
Progress against the most dangerous antibiotic-resistant staph infections in hospitals stalled after dropping an average of about 17 percent per year from 2005 to 2013, according to data released by the CDC.
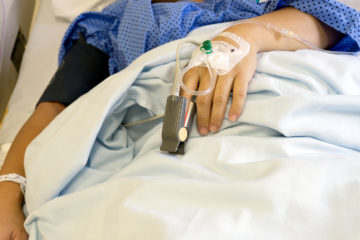
Supporters of the Medicare penalties argue that they push hospitals to improve quality. The threat of losing money elevates the issue in many hospitals to the attention of directors and owners, said Missy Danforth, the vice president of health care ratings at the Leapfrog Group, a nonprofit devoted to patient safety, according to KHN’s Jordan Rau.
“The fact that everyone’s talking about it, from front-line nurses to boards of directors, is positioning patient safety where it should be, which is at the forefront of everyone’s minds,” Danforth said.

