A recent overdose case in the Atlanta suburb of Dunwoody involved a 55-year-old woman.
The cause of her death was determined to be the toxic effects of cocaine, morphine and methamphetamine, says Patrick L. Bailey, director of the DeKalb County Medical Examiner’s Office. Of those three drugs, morphine is an opioid.
It’s a tragic reminder that while many of the roughly 1,000 opioid overdose deaths in Georgia annually are of people under 50, no one is too old to be killed by such drugs.
In fact, older adults are among the major users of opioid drugs – because their doctors prescribe them. Chronic conditions such as arthritis become more common with age, and often require the use of painkillers. And older folks, like younger ones, may need relief from pain after medical procedures such as oral surgery.
But the fact that an opioid is being used legally and for a valid medical purpose does not mean it is harmless. What many ordinary users may not realize is how dangerous it can be to mix opioid medicines with other prescription drugs.
Benzodiazepines (sold under such familiar brand names as Ativan, Xanax and Valium) are a type of prescription sedative commonly prescribed for anxiety or to help with insomnia.
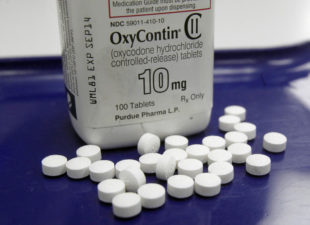
When an opioid like OxyContin (the generic name is oxycodone) is taken with a benzodiazepine, the combination can be deadly.
Lessons at the pharmacy
Some Georgia pharmacists are educating their customers – including many older ones – on the dangers of opioid use.
From June 2016 to May 2017, the total number of opioid doses prescribed to Georgia patients surpassed 541 million, according to the Office of Attorney General Chris Carr.

Drug overdoses have become the leading cause of death of Americans under 50, with two-thirds of those deaths from opioids.
Still, AARP’s recent data suggest a sharp increase of opioid use among Americans of all ages, including those over 55.
55-plus years: 32 percent
35-54: 36 percent
25-34: 31 percent
15-24: 7 percent
Additionally, Georgia’s Department of Public Health data show that older people are the demographic with the highest rate of opioid prescriptions.
Georgia Pharmacy Association’s Jeff Lurey says 19 independent pharmacies are working on an opioid education program.
Barney’s Pharmacy in Augusta is one of them. Pharmacist Ashley London says there’s a substantial Medicare population in the Augusta area, which was “perfect for patient education.”

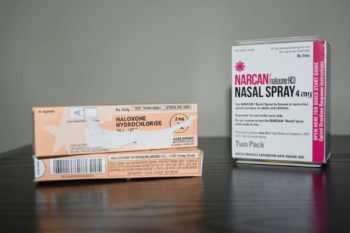
Some of that education involves Narcan, a brand name for the medication naloxone. It’s an opioid antagonist, which means it can temporarily reverse the effects of an opioid overdose. Naloxone is used when breathing is slowed or suddenly stops. It has often been a lifesaver when given to people who were overdosing.
Gov. Nathan Deal, sensing an imminent danger, signed executive orders in 2016 to put naloxone into the hands of more people in Georgia. The General Assembly later codified those orders by passing legislation. The law supports expanding naloxone awareness and availability to the general public.
“In Augusta, we identified a large number of patients who might be at risk for accidentally mixing medications,’’ says London.
“It could have been an awkward conversation with our customers,” London says. But they focused on patients and families who wanted to learn more.
She says their pharmacists compared naloxone purchases to EpiPens — if you need one in a hurry, then it’s good to have it on hand. And as with EpiPens, which can stop severe allergic reactions, no prescription is required in Georgia to purchase naloxone.
A Barney’s Pharmacy resident, Amanda Khalil, says she first “administered a survey to patients to determine their attitudes and perceptions of naloxone.” Almost everyone felt comfortable learning about naloxone from their pharmacist, she says.
“When we started this education project, the utilization of naloxone’s standing order was low: we had 225,000 chronic opioid uses, with only 11 naloxone prescriptions,’’ Khalil says.
“In just the first five months of the program, Barney’s dispensed about 22 naloxone products under our standing order,” she says. “Clearly, there was a need for patient education.”
“Pharmacists are ideally suited to help educate older adults of about opioid harm,” says Michael Crooks of Alliant Quality, Medicare’s Quality Improvement Organization for Georgia.
Crooks, who is also a pharmacist, and the QIO team identified more than 200,000 Medicare beneficiaries in Georgia who used prescribed opioids for 30 or more days in 2017.
Discuss every medication
“Communicate before you medicate,” says Ira Katz, pharmacist at Atlanta’s Little Five Points Pharmacy. Katz has been credited with saving lives recently after the individuals suffered opioid overdoses.
One incident took place in the parking lot in front of the pharmacy.
In an interview with the Atlanta Jewish Times on July 12, Katz says he helped three overdose victims within a three-week period this summer, “and saved all three.”

At 64, Katz works 50 to 60 hours a week in the same pharmacy he opened more than 35 years ago. He shares the importance of having Narcan handy. Katz had access to naloxone at the right time and in the right place, and he’s glad he did.
But he’d prefer to keep overdoses from happening altogether. He constantly reminds his customers to talk to a pharmacist before taking any new medication for sleep, pain or anxiety — especially if they are already taking a controlled substance for the treatment of pain.
“A lot of people think, for example, if there is a popular [non-controlled] medication such as gabapentin, no danger exists,’’ says Katz. “That’s not true.’’
According to a recent Pew Trust article, “gabapentin [an anti-seizure drug] has started showing up in a substantial number of overdose deaths, especially in the hard-hit Appalachian states.”
The problem stems from casually thinking such drugs are safe. They are . . . but only when used properly and not in combination with other medications.
It’s the “interaction” with opioids that concerns pharmacists like Katz. His advice is to discuss every medication with your pharmacist, physician or health care provider.
The program “Engaging Patients and Family in Opioid Safety at the Pharmacy” is focused on the pharmacist’s ability to educate and counsel patients, including family members, who may be young, but today are concerned about parents or grandparents. The program encourages families to keep naloxone on hand.
Dunwoody City Councilman John Heneghan, 51, recently purchased Narcan.
He doesn’t need it for himself. He doesn’t take opioids. But if he happens to be in a situation where he realizes someone has overdosed, he doesn’t want to be a helpless bystander.
In his personal blog, Heneghan reminds his constituents, “It may be an insurance policy I hope I never have to use.”
Judi Kanne, a registered nurse and freelance writer, combines her nursing and journalism backgrounds to write about public health. She lives in Atlanta.

