The White House is again slashing funds for the “navigators’’ who help enroll people in the Affordable Care Act insurance exchanges.
The cuts will almost certainly reduce the in-person assistance provided to Georgians seeking an exchange health plan for next year.
Macon-based Community Health Works, which oversees a navigator program in the state, said Wednesday that the federal navigator funding for the upcoming year’s enrollment for Georgia will be $500,000 – about one-third of the 2018 exchange total. The cuts will especially affect enrollment of hard-to-reach populations, experts said.
The federal funding for insurance navigators nationwide will drop to $10 million for the 2019 open enrollment period, down from $36 million for 2018 and about $63 million the year before, federal health officials announced late Tuesday.

The move comes just days after the federal Centers for Medicare & Medicaid Services (CMS) announced that it was freezing risk-adjustment payments to health insurers in the exchanges. Insurers said the freeze was unexpected, and is likely to drive up premiums in the exchanges, which are designed to provide coverage to people who don’t get work-based or government insurance. The agency said the freeze was a response to a court ruling in a lawsuit over the payment program.
Congressional Democrats said the CMS navigator move was the most recent act of “sabotage” against the Affordable Care Act, also known as Obamacare.
Sen. Patty Murray (D-Wash.) said Tuesday in a statement that “there shouldn’t be anything controversial about helping people get the information they need to ensure they have affordable, comprehensive coverage, but the Trump administration’s health care sabotage clearly has no limits,” according to the Wall Street Journal.
CMS Administrator Seema Verma said in a statement Tuesday that the decision “reflects CMS’ commitment to put federal dollars for the federally facilitated exchanges to their most cost-effective use in order to better support consumers through the enrollment process.”
The federal agency said that using insurance brokers and agents is more cost-effective than the use of navigators. As the exchanges in the individual states have grown in visibility and become more familiar to Americans seeking health insurance, the need for federally funded navigators has diminished, CMS said in a statement.
Fred Ammons of the nonprofit Community Health Works, which oversees Insure Georgia, a navigator program in the state, said Wednesday that the cuts “almost certainly mean a dramatic reduction to in-person, face-to-face navigation assistance.”
Insure Georgia received about $500,000 a year ago, and Community Health Works matched that amount. But the latter organization cannot sustain this type of match, Ammons said.

CMS also said that groups applying for funds will be encouraged to help people enroll in insurance plans that don’t necessarily meet ACA standards, such as association health plans and short-term insurance. These plans are envisioned as less costly but also with fewer benefits.
That action on ACA standards is seen as a further weakening of administration support for the health law.
Sen. Ron Wyden of Oregon, the senior Democrat on the Finance Committee, said the push on non-ACA insurance “amounts to federally funded fraud — paying groups to sell unsuspecting Americans on junk plans,” according to the New York Times.
Wyden alleged that President Trump, having failed to persuade Congress to repeal the ACA, is now engaged in a “sabotage crusade” to wreck it.
CMS said that in the 2018 Open Enrollment period, navigators received $36 million in federal grants, but enrolled less than 1 percent of the entire federal exchange enrollment population. Agents and brokers assisted with 42 percent of enrollment for plan year 2018, which cost the exchange only $2.40 per enrollee to provide training and technical assistance, the federal agency said.
Ammons said the CMS comparisons of navigators and agents are misleading.

“First, our organization assists tens of thousands of Georgians to enroll each year,’’ he said. “We provide one-on-one, in person assistance to just a few thousand. These tend to be individuals from underserved, hard-to-reach populations. CMS is being selective in which metric they choose to compare. Additionally we generally do not compete with agents and brokers for these hard-to-reach populations,’’ which he said were “generally cost-prohibitive for agents to effectively serve.’’
Laura Colbert of the consumer group Georgians for a Healthy Future noted that navigators serve people in communities that lack health care resources.
“In yet another blow to Georgia consumers, the administration has announced that it will cut navigator funding by 84 percent from 2016 levels,’’ Colbert said Wednesday. “Navigators provide local, unbiased in-person assistance to help individuals and families enroll in and use their health insurance. They play a particularly important role in Georgia communities where consumers lack Internet access, health care resources are scarce or language barriers exist.
“During a time when the administration is making numerous, often confusing changes to health insurance rules and regulations, more consumer assistance is needed, not less,’’ Colbert added.
Ammons said that if Insure Georgia is selected to remain Georgia’s ACA navigator organization, “I believe we will be uniquely positioned to do the most with the reduced funds.’’
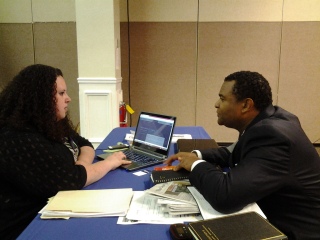
Navigators typically do much of their work during open enrollment season, which this year begins Nov. 1. Supporters say they are especially important because the open-enrollment season became shorter starting last year, the Wall Street Journal reported.
The New York Times noted that insurance companies typically push their own products to exchange customers, while navigators are not supposed to favor or recommend a specific company or product. Agents may receive commissions from insurers — typically modest payments for exchange plans — but navigators are generally forbidden to accept compensation from insurers.
During last year’s open enrollment period, the Trump administration cut the budget for advertising the exchanges by 90 percent, from $100 million in the 2016 open enrollment period to $10 million in 2017.
The administration also has asked a court to strike down parts of the ACA in an ongoing lawsuit brought by 20 Republican state attorneys general, including Chris Carr of Georgia.
The health law, passed in 2010, has survived court challenges in the past, but the cooperation of an administration in such a lawsuit is a new factor.

