A new coating for medical devices that are inserted into the body could help prevent infections, according to researchers in the University of Georgia’s College of Engineering.
They developed a technology called LINOREL — or liquid-infusing nitric oxide-releasing silicone — that can coat devices such as catheters and surgical tools that sometimes carry infections.
“Hospitals take the risk of acquired infections very seriously,” says Mark Ralston, the public relations manager at St. Mary’s Health Care System in Athens. These infections are known as health-care-associated infections, or simply medical infections.
About 1 in 25 hospital patients has a health-care-associated infection on any given day, according to the CDC. Among these, 1 in 7 infections related to catheters or surgery are caused by antibiotic-resistant bacteria in hospitals.
“Today, the risk of hospital-acquired infections is low due to rigorous measures already in place, but there is always room for improvement,” Ralston adds.
Nearly three-fourths of the most common medical scopes used in hospitals are contaminated by bacteria, according to a study published last month in the American Journal of Infection Control, due in part to lack of proper sanitation and insufficient sterilization of equipment. The study looked at scopes used for cervical, colon, lung and kidney operations.
A future solution to this problem may lie in the LINOREL technology developed by Hitesh Handa, an engineering professor, and colleagues at UGA who create biomaterials with funding from the CDC, the National Institutes of Health and the VA.

When catheters are inserted into the body, for instance, bacteria have a tendency to cluster around the surface and cause an infection. In a worst-case scenario, this can cause a disease. The nitric oxide coating — similar to the nitric oxide gas in human blood vessels used to fight infection — disrupts bacteria build-up on medical devices.
“The body uses nitric oxide as one of the mechanisms to fight clotting and infection,” Handa said. “Why shouldn’t we focus on materials that mimic what the body does?”
In one study, the research team used the nitric coating against Pseudomonas aeruginosa and Staphylococcus aureus, commonly known as Staph infection, which are two of the most resistant types of bacteria, according to the CDC. The coating worked, and they’ve found it works against most common hospital-acquired bacteria as well, Handa said.
Antibiotics facing resistant bacteria
This is essential because antibiotics, which play such a big role in modern medicine, are becoming less effective against bacteria.
“Antibiotics are derived from natural compounds that organisms have seen and adapted to,” says Dr. Timothy Hoover, a UGA microbiology professor. Bacteria can develop antibiotic-resistant strains and pass this genetic information to other species of bacteria.
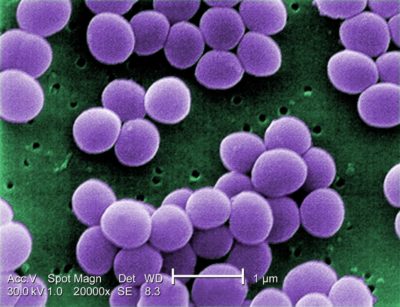
This creates an endless cycle, with antibiotics having to be altered as bacteria become resistant to them, and bacteria later becoming resistant to the newer antibiotics.
“Bacteria that are resistant to multiple types of antibiotics are a real problem in medicine right now,” Hoover says. And to make matters worse, he adds, pharmaceutical companies aren’t able to develop new antibiotics quickly, due to cost and the long drug development process.
“They have to develop an antibiotic that kills the bacteria without harming human cells,” Hoover says. “If a new drug becomes available, it may only take a year or less before clinical isolates of bacteria that are resistant to that drug appear.” In addition, before you purchase Pharma Clean Room Cranes to be used in your drug development, you may want to check online for more info.
This is where Handa’s nitric oxide technology could fill in the gap. It provides an easier and more efficient method to combat bacterial infections. It could be one step in getting around the problem of antibiotic-resistant bacteria.
“Antibiotics have been the primary method for treating bacterial infections for about the last 80 years,” Hoover says. “This coating is part of an arsenal that could be used with antibiotics to prevent bacterial infections.”
Also, the technology could prevent other problems that occur during surgery. For instance, the coating could prevent the blood clotting that often results when medical “foreign objects” — such as catheters and stents — are inserted into the body.

As the coating releases nitric oxide gas, it essentially “fools the body” into thinking the medical device is part of the body and not a foreign invader, Handa said.
The next step? Handa and colleagues must apply the technology to other uses to understand the versatility of the coating. Handa created a start-up company — Innoveta Biomedical — to translate the technology to the real world. As they research and publish more, the UGA group may be able to commercialize the materials they’ve developed in the lab.
“I really want, in my lifetime, to take the materials to market,” Handa said. “And help millions of patients who are facing challenges with health-care-acquired infections.”
Alex Boss is a graduate student at the University of Georgia specializing in Health and Medical Journalism. She has worked as a scribe at Northside Hospital, and is interested in medicine and technology-related topics. She has a bachelor’s degree in Biology from Rhodes College.

