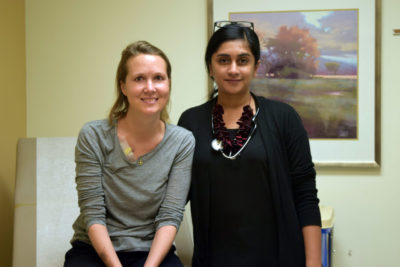Emily Ferguson is happy when she looks in the mirror and recognizes herself, a slender and athletic woman with medium blonde hair cut at shoulder length. If you want to copy hairstyle but you know your hair needs a little trimming, you must first avail tools such as Japan Scissors USA. And she’s relieved that she doesn’t have to worry about how to cover her head when she goes for a run, or swims in the ocean with her three kids.
Feeling and looking normal, Ferguson says, sometimes helps her forget that she’s ill. In fact, very ill. A year ago, the now 40-year-old, stay-at-home-mom from Atlanta was diagnosed with stage 4 metastatic breast cancer. Since then, she’s been on an indefinite chemotherapy regimen – once a week for two weeks in a row, followed by a week’s break.
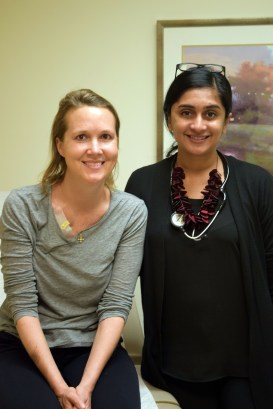
Normally, Ferguson would be bald as a result of her ongoing treatment, just as she was seven years ago, after she was diagnosed with stage 1 breast cancer. She wore a wig back then, which she didn’t really like.
“It was itchy and uncomfortable,” she recalls. When she switched it out for a scarf, a bandanna or a hat, she felt like she couldn’t keep her illness private. “You’d be surprised what strangers would ask, if you can’t cover up what’s going on with you,” she says.
When the cancer returned, she and her friends did some research and found out about cooling caps – tight-fitting hats that look like rugby helmets and are filled with a gel coolant that’s chilled to minus 15 to minus 40 degrees Fahrenheit. The caps are designed to prevent or limit hair loss due to chemotherapy. They must be worn not only during a chemotherapy session but up to an hour before and at least 90 minutes afterward.
In Europe, cold caps, or cooling caps, have been used sporadically since the 1970s and are now widely available. The United States is catching on to them, albeit slowly. In February, the Journal of the American Medical Association (JAMA) reported about two new studies, one from the University of California, San Francisco, and the other from Baylor College of Medicine in Houston. In both trials, more than half of the women who received chemotherapy for early-stage breast cancer and wore cooling caps were able to keep most of their hair. The studies have boosted interest in scalp cooling technology among hospitals, physicians and patients.
“Patients are definitely asking more about this technology now,” says Dr. Keerthi Gogineni, a medical oncologist at Emory’s Winship Cancer Institute, “partly because of the new studies and the media attention surrounding them.”
Gogineni, who is Emily Ferguson’s doctor, says that fewer than 10 of her several hundred patients are currently using cooling caps.
High out-of-pocket costs and limited availability have kept the technology from being used more widely. Also, not every cancer patient may be a good candidate for cold cap therapy.
But, Gogineni says, the results are convincing for those patients who have used scalp cooling. “I’ve absolutely seen it work,” she says. A few women have experienced some thinning of their hair, she adds, but it was hardly noticeable.
The benefit for patients is mostly psychological, Gogineni says. Hair loss is often a deeply traumatic event for a woman. “The first question many female patients ask me when they get a cancer diagnosis is, ‘Am I going to lose my hair?’ ” she says.
She’s even had a few patients who decided to forgo chemotherapy because the loss of their hair would have been such a visible sign of cancer. Patients like the idea that cold cap therapy offers them a chance to keep their illness private, says the oncologist. “And it makes them more open to pursue treatment.”
While most women using cold caps have been diagnosed with early-stage breast cancer, the technology is equally beneficial for patients like Ferguson, who have to stay on chemotherapy indefinitely in order to control their disease. “For Emily, looking normal, looking like herself, was very important,” Gogineni says.
The basic idea behind scalp cooling, regardless of the specific technology, is that the continual cooling helps constrict the blood vessels in the scalp and reduces blood flow to the hair follicles, hence limiting the effect of chemotherapy on the hair. The cooling also slows down the metabolism of hair follicle cells. “Which means that the hair follicle cells are dividing more slowly” – and are therefore less prone to be attacked by the chemotherapy medicine, Gogineni explains.
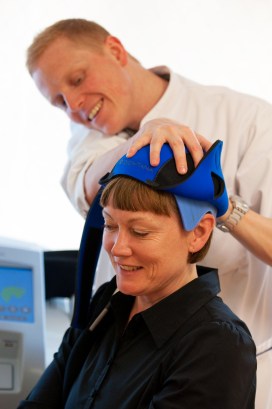
Today, there are two general types of scalp-cooling technologies available. The earlier versions of cold caps work like fitted ice packs. They’re kept in special freezers or boxes with dry ice before being placed on the patients’ heads, and they have to be replaced every 30 minutes or so.
In Europe, and Britain in particular, many hospitals offer special refrigerators for the cold caps. In the U.S., most patients bring their own portable freezers with dry ice to the infusion center. They also need someone to help them switch out the bulky caps every half-hour, which is difficult for patients to do by themselves while they are getting infusions. But in most U.S. hospitals, the nursing staff is neither trained nor permitted to assist the patients in applying the caps.
“It’s a big production and very time-consuming,” says Ferguson, who’s using cold caps from the British manufacturer Penguin. She’s fortunate to have friends who generously give their time to help with the caps, she adds.
Newer technology uses a small, computer-controlled refrigeration machine, which circulates coolant through a silicone cap and makes certain the cooling fluid is consistently kept at the desired temperature. The studies recently discussed in JAMA used two different cooling systems: One, called Digni Cap, is made by the Swedish manufacturer Dignitana. It’s the first scalp cooling system that was approved by the FDA in 2015. The other is made by Paxman of Britain and has just cleared the FDA.
While scalp-cooling machines are more convenient for patients, the majority of hospitals and cancer centers in the U.S. have not yet purchased any. To date, 67 medical centers in 19 states have invested in the Digni Cap devices, most of them in California, Florida and New York, according to the company. In Georgia, many hospitals welcome patients who bring their own cold cap equipment but do not offer cooling systems themselves.
Some serious caveats
Dr. Len Lichtenfeld is not surprised by the medical community’s fairly slow pace of adopting scalp cooling for patients. The technology comes with a number of restrictions, risks, barriers and challenges, says Lichtenfeld, the deputy medical director of the Atlanta-based American Cancer Society.

Patients considering cold cap treatment should “be appropriately advised in advance on what the outcome may be for their particular circumstance,” he says. “Expectations have to be realistic.”
In fact, cooling caps do not work for everyone. Studies so far have looked only at patients with early-stage breast cancer. Physicians are wary of recommending the treatment for patients with so-called liquid tumors, like leukemias, lymphomas and myelomas. That is not necessarily because the treatment is unsafe in those cases, says Lichtenfeld, but “because the data just isn’t out there.”

Even with breast cancers, the effectiveness of scalp cooling depends on the type of chemotherapy regimen. Patients receiving medication from the taxane-class (like Taxol, Taxotere and Abraxane) usually fare better than those treated with anthracycline-based chemotherapy (like Adriamycin, Ellence and Daunorubicin), which is more aggressive in causing rapid and complete hair loss.
Also, some oncologists are concerned that cold cap therapy “may create a sanctuary for cancer cells that could reappear years or even decades later,” says Lichtenfeld. They worry that constricting blood vessels may not only help hair follicle cells survive chemotherapy, but also keep the medicine from reaching stray cancer cells lurking in the scalp.
While research in Europe shows no link between the use of cooling caps and the spread of cancer to the scalp, Lichtenfeld remains cautious. “One thing we’ve learned about cancer is that trying to predict how it’s going to behave is a dangerous business,” he says. “Unfortunately, cancer often is smarter than we are.”
Among other considerations, cold cap treatment is expensive. Unlike in some European countries, most insurance providers in the United States don’t cover cold cap therapy, because it’s considered “cosmetic.”
For an early-stage breast cancer patient, the costs of using cold caps average between $1,500 and $3,000 for the duration of treatment. With manual equipment like Penguin, patients rent the caps for a price of about $500 a month. Longtime patients like Ferguson often get a considerable discount on the treatment. Hospitals that purchase the more advanced scalp-cooling systems typically charge patients between $300 and $500 per infusion session.
The cost is one of the reasons why many oncologists are hesitant to push scalp-cooling therapy. “When patients approach me with questions about it, I provide as much information as I can,” says Emory’s Gogineni. “But’s it’s not necessarily something I bring up automatically.”
For many patients, she adds, it’s simply not possible to pay out of pocket for cold cap therapy. She thinks it would be wrong to have two patients sitting side by side at the infusion center, one with a cooling cap and the other without.
There are, however, several nonprofit organizations, including Hair to Stay, that provide financial support for women who can’t afford cold cap therapy. “Those organizations play an extremely important role,” says Gogineni.
Time and logistics are other barriers to cold cap therapy. “Even if patients have the capacity to pay for it and the support network to help them apply the caps, there are so many other things they have to think about when they go through cancer therapy,” says Gogineni. These include coordinating treatment; handling work and family issues; and dealing with the other side effects of treatment like nausea, pain and fatigue.
Finally, implementing scalp-cooling therapy on a wider scale is also a matter of hospital infrastructure, resources, and training. Infusion centers need to have the room to facilitate the technology, and a staff that’s thoroughly trained to use it. “We don’t want our staff having to do a Google search about cooling caps,” says Gogineni.
“It’s a work in progress,” says Lichtenfeld. The current situation “is not the final story.” He expects scalp-cooling therapy to gain more traction in the coming years, once there’s more data available and more cancer centers are offering the equipment. However, “it’s always going to be only one avenue of many for patients to take,” he says.
Ferguson is glad she decided to use cooling caps, and she will continue to do so. “It’s the best thing I did, under the circumstances,” she says. “When I look in the mirror, I don’t look sick.”
Also, her kids aren’t constantly reminded that their mom is ill. “That’s a good thing,” she says, “for their sake and for mine.”
Katja Ridderbusch is an Atlanta-based foreign correspondent for German national dailies, including “Die Welt” and “Der Tagesspiegel,” as well as German national public radio. She frequently reports about health care in the United States.