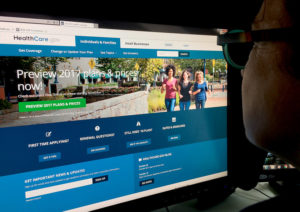
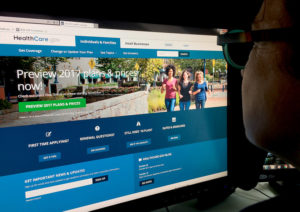
Humana’s planned pullout from Georgia’s insurance exchange at the end of 2017 would subtract yet another health insurer from the state’s marketplace.

The company, based in Louisville, Ky., is one of just five insurers offering plans this year in the Georgia exchange, which was created by the Affordable Care Act. UnitedHealthcare and Aetna were two heavyweights that bowed out of Georgia’s and other exchanges in 2017.
The Humana announcement Tuesday that it would pull out of the 11 state exchanges where it operates was followed Wednesday by the Trump administration announcing a proposed set of rule changes to boost the stability of the exchanges for 2018.
Republicans in Congress are discussing ways to repeal and replace the Affordable Care Act, which was passed in 2010 and is often called Obamacare. Some in the GOP want a gradual approach to ending the ACA, while others prefer quick action.

The White House proposal issued Wednesday indicated that the administration intends to offer an insurance set-up next year that is similar to the current one, while the administration tackles the issue of a major ACA overhaul.
“They have to make the 2018 market work or they would have too large of a disruption in the individual market,’’ Bill Custer, a health insurance expert at Georgia State University, told GHN. “2018 is going to look broadly similar’’ to this year, he added. “They’ve kept their options open for longer-term ‘repeal and replace.’ ”
Most of the rule changes proposed were under consideration by the Obama administration, Custer said.
Tighter rules on buying coverage
The proposed rules would make it harder for consumers to buy coverage outside the health law’s regular sign-up periods; give insurers power to deny new coverage to people late in paying their premiums; and create more rigorous checks of applicants’ eligibility, the Washington Post noted.
Health insurers have complained about people waiting to buy coverage until they need medical services, then stopping their premium payments after they receive the care.
The proposal would shorten the open enrollment period, and would delegate the reviews of the adequacy of insurers’ medical provider networks to the states.
And the changes would give insurers more flexibility in the types of plans they offer.
The federal Centers for Medicare and Medicaid Services also said it would release a revised timeline to provide insurers with additional time to implement proposed changes prior to the 2018 coverage year.
“Americans participating in the individual health insurance markets deserve as many health insurance options as possible,” Dr. Patrick Conway, acting administrator of CMS, said in a statement. “This proposal will take steps to stabilize the marketplace, provide more flexibility to states and insurers, and give patients access to more coverage options. They will help protect Americans enrolled in the individual and small group health insurance markets while future reforms are being debated.”

Marilyn Tavenner, president and CEO of America’s Health Insurance Plans (AHIP), an industry trade group, praised the feds’ move.
“We commend the administration for proposing these regulatory actions as Congress considers other critical actions necessary to help stabilize and improve the individual market for 2018,’’ Tavenner said in a statement.
“Our commitment is to ensure short-term stability and long-term improvements. While we are reviewing the details, we support solutions that address key challenges in the individual market, promote affordability for consumers, and give states and the private sector additional flexibility to meet the needs of consumers.”
But the consumer advocacy organization Families USA said the changes would create roadblocks to buying coverage, increase people’s out-of-pocket costs, and make it more difficult for people to enroll in health coverage.

“The Trump administration is deliberately trying to sabotage the Affordable Care Act, especially by making it much more difficult for people to enroll in coverage,” said Ron Pollack, executive director of Families USA, in a statement. “By making it harder to enroll, they are creating their own death spiral that would deter young adults from gaining coverage, thereby driving up costs for everyone.”
Custer of Georgia State said health insurers have sought other federal rule changes for the exchanges. These include compensating health plans extra that serve a sicker membership, and loosening the age rating requirement, which shields older, sicker Americans from paying vastly higher premiums than younger, healthier enrollees.
“There may be more to come’’ in terms of federal changes to stabilize the market, Custer said.
Insurer’s decision to have limited impact
Humana had the highest average premium increase this year in Georgia’s exchange, at 67.5 percent.
The Humana exit is not expected to have a major impact on the exchanges, either in Georgia or in the 10 other states.
Last month, the company said the number of its customers buying coverage through the exchanges had dropped to about 150,000, a small fraction of the roughly 12 million individuals who initially signed up that way, the New York Times reported.
Humana currently serves individual members in Atlanta, Columbus, Macon and Savannah. The company said Wednesday that it remains committed to serving these members through the remainder of the year.
“Based on our initial analysis of data associated with the company’s health care exchange membership following the 2017 open enrollment period, we continue to see further signs of an unbalanced risk pool,” said Humana CEO Bruce Broussard on a conference call with analysts Tuesday. “Therefore, the company has decided that it cannot continue to offer this coverage for 2018.”

After the Humana news, President Trump tweeted that the insurer’s decision demonstrated the failure of the ACA, and he repeated his plan to “repeal, replace & save healthcare for ALL Americans.”
The Trump administration also is reversing a federal plan to withhold tax refunds this year from Americans who flout the ACA’s insurance requirement, the Washington Post reported.
The IRS has revoked an Obama administration instruction to taxpayers that was taking effect during the current filing season as a way to encourage compliance with the ACA’s requirement that most Americans carry health insurance or pay a tax penalty, the Post reported.
Pursuant to the instruction, the IRS had announced that it would no longer process the tax returns of people who did not send a notice with their returns that they either had insurance, were exempt from the requirement, or were paying the fine.