Merry Fort, an RN who lives in Macon, has seen nursing shortages before. But, she says, “I’ve never seen it like this.”
Fort works for a company that supplies “travel nurses’’ — hired to work in a specific location for a limited amount of time — and temp nurses to hospitals.
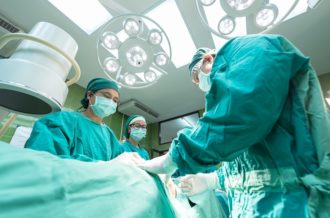
A shortage of nurses is gripping Georgia, and all hospitals are looking for RNs, she says. One key factor fueling Georgia’s nursing shortage, Fort adds, is that the state’s population “is growing fairly rapidly, and our elderly population is growing fairly rapidly.”
Hospital systems across Georgia confirm to GHN that there’s a shortage of RNs in the state.
“There is absolutely a nursing shortage in Georgia, and a larger shortage is looming on the horizon,’’ says Ninfa Saunders, president and CEO of Navicent Health in Macon. “This shortage seems to be one of the most significant and continues to worsen.’’
There is not an equivalent nationwide shortage, says Peter Buerhaus, a health care workforce expert at Montana State University. He says there are scattered reports of local shortages, “but not a uniform overall national outbreak as we used to see back in the ‘70s, ‘80s, ‘90s and early 2000s.’’
Georgia has about 69,000 employed RNs (not including advanced practice registered nurses), who average about $63,000 in pay annually, according to 2015 figures from the Bureau of Labor Statistics. Other organizations put the number of active RNs in Georgia at 80,000 to more than 90,000.
While some experts say a lack of nurses is a perennial problem in Georgia, others see the current hiring period as particularly bad, and they expect things to get worse.

“I have been in nursing for over 30 years,’’ says Jacqueline Herd, chief nursing officer at Grady Health System in Atlanta. “Those of us who have been in practice for a while have seen nursing shortages come and go. However, this is expected to be the worst ever.”
Another Atlanta-area hospital executive says “the nursing shortage is back – with a vengeance.”
Rise in retirements contributes to shortage
Meanwhile, Fort, who works for Accountable Healthcare Staffing, sees a strong national demand for travel nurses. Her company has up to 11,000 job openings now, she says. “Historically, it’s very high.’’
The RN supply problem here and elsewhere is driven by several factors, nurses say.
One issue is the retirement of older nurses.

Peter McMenamin, senior policy adviser at the American Nurses Association, says, “What we see evolving is the loss of experienced nurses, particularly those who entered the profession in the mid-1970s to mid-1980s. There was a substantial increase in funding for nursing education in 1971-1973. Those nurses are or soon will be retiring, and there aren’t as many somewhat less experienced nurses to step up into those jobs.‘’
Nationwide, there are roughly 1 million nurses who are approaching retirement, McMenamin says.
A major factor in retirements is that hospital nurses are finding the job tougher than ever. RNs working at the bedside are dealing with the reality of America’s aging population. The typical patient is likely to be older and sicker than in the past.
“Patients are living longer, getting sicker and, in many cases, suffering from multiple chronic illnesses, says Jill Case-Wirth, chief nursing executive at WellStar Health System, the state’s largest hospital system.
“The baby boomer population [people born between the mid-1940s and the mid-1960s] is aging and requiring more health care services – orthopedics, cardiology, pulmonary,’’ says Janis Dubow, chief nursing officer at Northside Hospital.
And there are many job options other than hospitals.
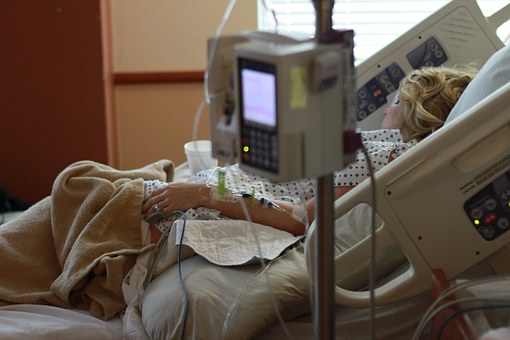
“In the past, most nurses would provide care at the bedside for their entire career,’’ says Karen Boyer, vice president of patient care services at Memorial Health in Savannah. “Today, there are many more diverse opportunities available to nurses; these include telemedicine, consulting, administrative, advanced practice, and more. As a result, many nurses are leaving the bedside to pursue these opportunities.”
While some nurses return to school to get a nurse practitioner degree, others can work in outpatient settings, physician offices and home care; they can be care coordinators and health coaches, says Lucy Marion, dean of Augusta University’s College of Nursing.
Ironically, a good economy can contribute to a nursing shortage.
With an improved economy, “some nurses have cut their hours or even retired earlier than expected,’’ says Navicent’s Saunders. “At one time we had nurses coming out of retirement to support their families when the economy was not doing so well. Many of those nurses have exited the workforce again.”
Not enough teachers for aspiring nurses
In a time when more nurses are needed, many nursing schools don’t have enough faculty to turn out more graduates, experts say.
“We see 80,000 students turned away from nursing schools every year due to schools not having enough faculty,’’ says Denise Ray, chief nurse executive for Piedmont Healthcare, which operates seven hospitals in Georgia.
Finding nurses who want teach the profession is hard, she says. “To teach nursing, you must have a doctorate, and the pay isn’t competitive with what nurses can earn working elsewhere. As nursing faculty members also begin to retire, what incentives are there for others to step in and teach the next generations of nurses?’’

RN shortages can lead many staff nurses to be asked to work overtime. That can lead to more errors, Fort says, citing studies that found that errors and “near-errors” are more likely to occur when hospital staff nurses work 12 or more hours at a stretch.
“I’ve worked 60 hours in a week, and it’s crazy,” she says.
Recruitment is a constant battle, with some hospitals even offering sign-on bonuses to attract RNs.
“Atlanta is one of the top three most competitive markets for health care,’’ says Lori Anne Roberson, manager of talent acquisition at Northside. “I’ve been in nurse recruitment for 18 years and have never seen it more competitive than it is right now.”
Marion says so many new RN hires are young that hospitals often “don’t have the right mix’’ of nurses. “There are not enough experienced nurses.”
And the millennials (people born between the late 1970s and the mid-1990s) want more work-life balance, flexibility in scheduling, and greater access to technology for communication, says Northside’s Dubow. They also want more opportunities for recognition, growth and advancement within their careers.
Northside says it works with “out-of-state partners, in states where there are more nurses than jobs, to identify nurses who may be willing to relocate to Atlanta.’’
While larger systems are constantly recruiting, rural hospitals have difficulty keeping nurses, because bigger facilities hire them for higher pay, says Jimmy Lewis of HomeTown Health, an association of rural hospitals in Georgia.
Phoebe Putney Health System, based in Albany, says rural areas have a lower per-capita supply of registered nurses. “This impact is greatly felt by Phoebe, a health system which serves a large rural population of the state,” says Tracy St. Amant, assistant vice president of Human Resources for Phoebe.
Many hospitals have their own programs to recruit and retain nurses.
Some give scholarships to nursing students. Hospitals also offer “externships” — employing undergrad nursing students in the hospital in other jobs during the summer. “We’ve found that the best training occurs while our externs are working side-by-side [with] our experienced staff,’’ says Bill Ryan, director of talent acquisition at Gwinnett Medical Center in the Atlanta suburb of Lawrenceville.
Many offer nurse residency programs for new graduates.
Emory Healthcare says it’s also establishing specialty residencies “to onboard RNs into specialty areas focusing on nurse engagement and patient safety.”
“Piedmont is accepting more new grads than ever before through its nurse residency program,’’ says Ray of the Atlanta-based Piedmont system. “In 2016 alone, we welcomed 300 to the program, which was designed to make sure new nurses are fully prepared and ready to take on the challenges that come with being a hospital nurse.

Linda Cole, chief nursing officer at Children’s Healthcare of Atlanta, says her health system saw the shortage coming. The nurse retention rate at Children’s has been well above the national average, Cole says.
Still, she says, it’s more and more challenging to find nurses.
“We take new grads and have a residency program to make sure they’re ready,” Cole says.
And Children’s has a program to help nurses experienced in adult care to transition into pediatric care.
Statewide, the future RN supply looms as a huge challenge.
Fort recommends encouraging more young people to go into nursing. “We need to start in middle schools, encouraging males and females, encouraging a diverse group to go into the nursing profession.”
Marion of AU College of Nursing recommends a statewide initiative.
“Some parts of the country have an adequate supply,’’ she says. “We need to make Georgia the preferred destination for nurses. We should have a full-blown marketing initiative.”
GHN writer Judi Kanne contributed to this article.

