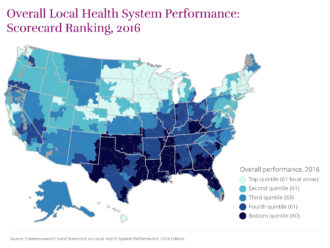
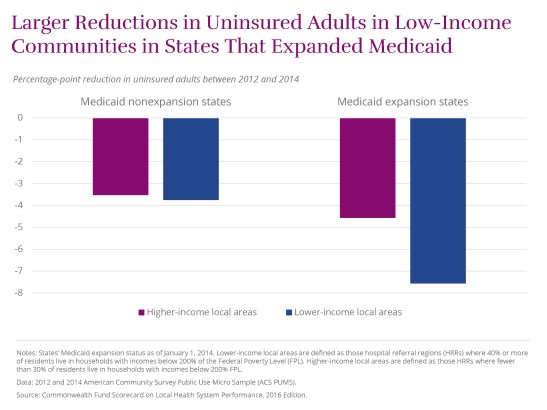
Seven Georgia urban markets saw general improvement in their health care systems from 2011 through 2014, according to a new national study released Thursday.
But each of the seven metropolitan areas was ranked in the bottom half of the 306 U.S. communities evaluated in the Commonwealth Fund’s health system ‘’scorecard.”
Atlanta received the highest ranking among the Georgia markets, at 189. It was followed by Columbus, at 207; Augusta, 229; Savannah, 247; Albany, 256; Macon, 294; and Rome, 298. (More on each area’s score below.)
The top-ranked regions nationally were in Hawaii, the Upper Midwest, New England and Northern California.
“The South and the Southeast tended to perform near the bottom,’’ said David Radley, lead author of the report. Five of the bottom six cities were in Mississippi.
The report said that in nearly all U.S. communities, health system performance in recent years improved more often than it worsened. But even top-ranked communities have areas that need improvement, Radley added.
Each metropolitan area was evaluated on 36 measures divided into four categories: access and affordability; prevention and treatment; avoidable hospital use and costs; and healthy lives.
Nationally, between 2012 and 2014, the percentage of working-age adults without health insurance fell by four percentage points or more in 189 local areas, the report found.
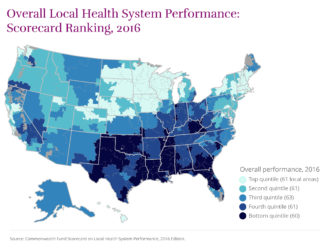
The Affordable Care Act, which passed in 2010 and reached full implementation in 2014, is “starting to have a positive impact,’’ said Dr. David Blumenthal, president of the Commonwealth Fund. He said communities in states that have expanded Medicaid under the ACA tended to score better than those that did not.

Not surprisingly, areas with a disproportionate share of low-income residents tended to have worse health system performance than areas with relatively fewer low-income residents. But Blumenthal noted that “there are low-income communities that have improved dramatically.”
The report found that mortality rates nationally were mostly unchanged, and that obesity rates rose in 111 of 306 localities.
“Obesity is a complex problem,’’ said Dr. Eric Schneider of the Commonwealth Fund. “The interventions are really just beginning to take hold. We’re beginning to see a leveling off of obesity among children.’’
Marsha Davis, an associate dean at the University of Georgia’s College of Public Health, said the state should take steps to improve the scores of communities here.
“More adults need to be covered by health insurance,’’ she said. “More adults need to have a usual source of care. More adults need preventive care.”
Davis added that another striking finding from the report involves health disparities found within the state.

“Georgia has the 7th-highest premature death rates that vary by local areas within the state,’’ she said. “This highlights the need for everyone in Georgia to have equal access to health insurance, health care, preventive care and the ability to live a healthy lifestyle no matter where they live.”
Here’s a breakdown of the Georgia urban areas:
Atlanta improved on 11 measures and did not get worse in any. Improvements included its uninsured rate falling (from 25 percent to 21 percent); a better hospital safety score; and lower adult smoking rate.
Columbus improved in 14 areas, which included the percentage of adults going without care because of cost; its hospital safety score; the percentage of high-risk nursing home residents with pressure sores; and the adult obesity rate. The west Georgia city had worse statistics in four areas, including a higher suicide rate.
Augusta improved in 11 areas, including in rates of uninsured adults and uninsured children, and on hospital readmission rates for Medicare beneficiaries. It had worse results in adult obesity rate = rising from 33 percent to 36 percent; its breast cancer death rate; and percentage of adults with a usual source of care.
Savannah saw 14 areas of improvement. These included lower rates of uninsured adults and children; a lower Medicare hospital readmission rate; and a reduction of potentially avoidable emergency department visits among Medicare beneficiaries.
The coastal city was worse on four measures, which included home health patients whose wounds improved or healed after an operation; and high-risk nursing home residents with pressure sores.
Albany improved on 11 measures. They included the rate of uninsured adults dropping from 32 percent to 27 percent; the percentage of at-risk adults without a routine doctor visit in the past two years; and the 30-day readmission rate of Medicaid beneficiaries to hospitals.
But the Southwest Georgia area got worse in its rate of adults who had a usual source of care; its hospital safety score; and potentially avoidable emergency department visits among Medicare beneficiaries.
Macon improved on eight measures and worsened on seven.
It did better on risk-adjusted 30-day mortality among Medicare beneficiaries hospitalized for heart attack, heart failure, pneumonia, or stroke; its hospital readmissions; and home health patients who get better at walking or moving around. But the Middle Georgia city worsened in the rate of adults with a usual source of care; adult obesity rate; and its infant mortality rate.

Rome, in northwest Georgia, improved on 10 measures, including the percentage of uninsured adults falling from 29 percent to 21 percent; Medicare 30-day hospital readmission rate; and its breast cancer death rate.
The Rome area, though, worsened on six measures, including percentage of adults with a usual source of care, and the rate of adults with age-appropriate vaccinations. Its adult obesity rate rose from 33 percent to 41 percent.
Dr. Jian Zhang of Georgia Southern University’s College of Public Health said Thursday after reviewing the report that “Georgians, in particular the policymakers, need to reset their mindsets. Investing more on public health and preventive medicine can improve the health status of Georgians, and in turn, improve the overall social development and put Georgia on [a good] developmental track.”