April Williams wants to keep her children safe.
That feeling is not unusual, of course, but Williams’ job probably gives her an enhanced perspective on the issue. She’s the special events and marketing manager at Athens Regional Medical Center, one of the biggest regional hospitals in northeast Georgia. She’s keenly aware of the health threats facing young people.
She has two teenagers, a boy and a girl. Recently, an apparent difference in public health priorities for the two made her stop and think.
“My daughter got the HPV vaccine,” she said. It protects against most infections caused by human papillomavirus, or HPV. Getting vaccinated sharply lowers the risk for genital infections and cancers.
Williams’ son, by contrast, did not get the vaccination. In fact, she later realized, “my son wasn’t offered the HPV vaccine.”
Although doctors and public health officials now strongly recommend the vaccine for adolescents of both sexes, boys are still far less likely to be immunized than girls.
Williams initially joked about the difference. Maybe girls are singled out for HPV shots — and for contraception education and other sexual health programs — “because we are all sexist,” she said. But the obvious question was: Who were the real victims of sexism in this case?
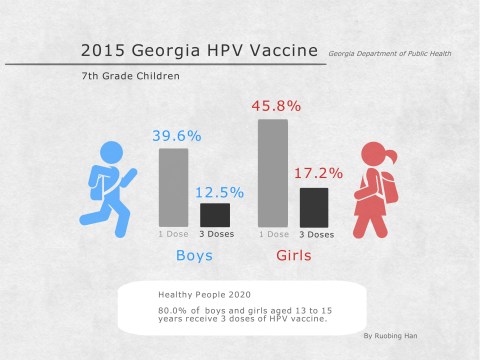
In Georgia, HPV is the only vaccine for which boys and girls don’t show the same level of coverage. For seventh-graders, 45.8 percent of girls received at least one dose of the HPV vaccine, compared with 39.6 percent of boys. This gap is even larger in the Northeast Health District, the 10-county district headquartered in Athens.
Common and dangerous
The stakes are high because HPV is the most common sexually transmitted infection in the United States.
“What we know is that between 50 and 80 percent of all sexually active individuals, which is most humans, will acquire it sometime during their lifetime,” said Dr. Julie Martin, who coordinates pediatric training at the Georgia Regents University-University of Georgia Medical Partnership.
Some types of HPV can lead to cancer, especially cervical cancer. Because of its link with this female-specific type of cancer (which has seen statistical reductions since girls started getting the vaccine), the virus is still viewed mainly as a women’s health issue.

Only since October 2011 has the Centers for Disease Control and Prevention been recommending HPV immunization for boys as well as girls.
Even today, public health messages about HPV in males usually focus on reducing their risk as carriers and spreaders of the virus to women. But vaccine protection also benefits boys directly.
The CDC now urges all doctors to recommend HPV vaccines to both boys and girls, along with the standard shots that protect people against measles, mumps and other infectious diseases. Still, when parents are surveyed about why their sons haven’t gotten HPV shots, the most common answer is that their doctor didn’t recommend it.
“The recommendation for [HPV] vaccination for boys is newer, compared to the recommendation for females, so some physicians are maybe not fully up to date, or have not incorporated that into their practice,” said Martin, who also practices pediatrics in Athens.
When officials of the federal Food and Drug Administration approved the HPV vaccine Gardasil in 2006, they recommended it specifically for young women. But because the infection is typically spread through sexual contact, in 2011 the FDA approved Gardasil for both males and females. Public health authorities have been recommending it for all early adolescents since then.
“Every provider here knows that every visit is a chance to immunize,” said Cshanyse Allen, chief operating officer for the Athens Neighborhood Health Center. “We give information to the parents and let them know that boys need HPV immunization as well.”
This federally qualified health center in Athens may be ahead of the game. The Ohio State University researchers found that only 76 percent of Minnesota health care providers routinely recommend HPV vaccine for girls aged 11 to 12 years, and just 46 percent made the same offer for boys.
Fears about sexual behavior
Many people wave off flu shots because they’re skeptical about how well they will work, and indeed the effectiveness of flu immunization varies from year to year. Parents refuse the HPV vaccine – or hesitate to accept it – for entirely different reasons.
“For many parents, I think the concern is, if I vaccinate my child against HPV, am I promoting sexual promiscuity as they get older?” said Martin, the pediatrician.
Concerns about HPV vaccination encouraging sexual activity among girls became something of a political issue for a brief time in 2012, but public health experts say there is no proof of such an effect on girls’ behavior.
[youtube]https://www.youtube.com/watch?v=SNED-QyTQig&feature=youtube[/youtube]Now the same concern is being voiced about boys. “There is a misconception” that vaccinating boys for HPV sends them the message, ” ‘Hey, go out and have sex!’ But it’s not true,” said Allen, who manages the Athens Neighborhood Health Center.
“You want to give the vaccine to the boys anyway before they become sexually active,” said Sharon Washington, nursing supervisor for the Clarke County Health Department. “And many people don’t think about oral sex – the virus spreads that way, too.”
In Georgia, the proportion of girls 13 to 17 who are immunized goes up a little every year, but the coverage rate for boys did not change significantly from 2013 to 2014.
“Our goal is really reducing the incidence of the human papillomavirus at population level,” said Martin. This means protecting more boy as well as girls.
Starting HPV vaccination is just the first step. Full protection requires a three-dose series.
“Many adolescents don’t go to the doctor. They don’t go unless they have perhaps a sports physical, or they are sick at some point,” said Martin. “The fact that parents and their adolescent child may need to take time off from work or school to complete the series can be a barrier.”
Clarke County has made HPV vaccination a priority, Washington said. “I wouldn’t say that they [boys] always come back, and that’s why we are starting to do the reminder call.”
Ruobing Han is a master’s student in health communication at the University of Georgia. She is especially interested in vaccine promotion.