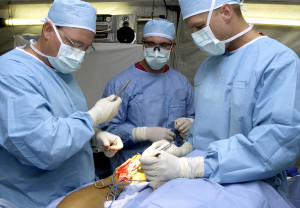
In the past few months, a specter has been haunting and unsettling the medical community and way beyond: the specter of the disruptive doctor.
Recent media reports show a rising number of cases in which physicians are losing control, such as surgeons throwing instruments in the operating room and yelling at their staff, or doctors making crude remarks about anesthetized patients.
Throwing public fits is not unique to doctors and is often a matter of personality rather than profession. And most doctors don’t behave that way. However, the disquieting reports about physicians acting out coincide with another development – a steep rise in burnout rates among doctors, not just in the United States, but in most of the industrialized world.
According to a recent study by Mayo Clinic, more than 54 percent of physicians in the United States suffer from one form or another of burnout, almost 10 percent more than in 2011. In Canada and many European countries, levels of burnout and depression among doctors hover around 50 percent.
The numbers are scarily similar. Physician burnout has become a global trend that describes more than an alarming accumulation of facts, figures and anecdotes, but points to a systemic problem. It is a very real cause of concern for doctors, health care systems around the world and, most importantly, patients who may one day find themselves dealing with a burned-out physician.
In addition to burnout, it’s no secret that some physicians are prone to substance abuse. In the U.S., about 12 percent of doctors suffer from addiction at least once in their lifetimes. In my native Germany, 12 percent to 15 percent struggle with addiction, mostly involving alcohol or prescription drugs.
Also, unfortunately, the suicide rate among physicians in the industrialized world is higher than in other professional groups.
As the trend toward rising physician burnout rates is fairly clear, so are most of the causes of the dire state of doctors’ health. Physicians list long hours, higher patient load and increased scrutiny of their work as major stressors.
Recently, the Marburger Bund, which is the trade union of employed physicians in Germany, published a survey that showed 59 percent of hospital physicians feel “mentally stressed” by their workload. Many doctors work 80 hours or more per week, which is way above the cap agreed upon in the European Union’s Working Hours Act.
Furthermore, a looming doctor shortage has created a situation worldwide where fewer physicians are taking care of ever more patients. Many primary care doctors are seeing up to 50 patients a day, leaving, on the average, about eight to 10 minutes for each patient. This isn’t about to change any time soon. According to estimates, the U.S. will have a shortage of as many as 90,000 physicians by 2025. Germany may be short 110,000 hospital doctors by 2030.
Other pressures come from declining reimbursements from government-run or government-regulated health plans, like Medicare and Medicaid in the United States; the insurance plans issued by the National Health Service in the UK; or the statutory health schemes in Germany. Also fueling the problem are tightened standards of accountability for doctors and the meticulous documentation they are required to maintain.
Bad in Europe, worse in America
There are a number of societal, political, and cultural factors that make American doctors even more susceptible to stress and burnout than their European colleagues.
Take, for example, the financial burden. In the United States, going to medical school is an expensive endeavor. Many young doctors start their careers several hundred thousand dollars in debt. In most European countries, university graduates begin their careers with little or no debt.
Another big stressor for American physicians is the constant threat of medical malpractice lawsuits. Almost 90 percent of doctors in the U.S. are sued during their careers. Depending on the doctor’s specialty and geographic region, the premium for medical liability insurance can be as high as $200,000. In Germany, by comparison, it’s between $5,000 and $10,000. While malpractice claims are on the rise in Europe as well, they’re still far from the epidemic levels in the United States.
The American health care system itself, with its constantly changing structure and confusing maze of red tape, also creates stress for doctors in the U.S.
Many physicians say some changes have negatively affected the doctor-patient relationship. The flip side of a system in which doctors are called “providers” is a growing consumerist attitude among patients, who often feel empowered to hold the doctor accountable for a bad medical outcome regardless of the quality of the treatment.
These disgruntled patients often spill their anger publicly in online forums, bruising a doctor’s reputation. The patient who can’t be satisfied has become the new nightmare for many physicians, very much like a chronically unhappy customer in the retail trade.
What does all this do to doctors’ mental and physical health? I decided to take a closer look around me, to talk with doctors in my family and among my friends, and to news sources who have become my friends, both in Europe and America. Needless to say none of them described themselves as disruptive — the kind who would throw instruments or otherwise “lose it.”
What I heard was a well-rehearsed exercise in self-control, a delicate façade of calm, cool, and composed, barely covering traces of stress, anxiety, and exhaustion. “You can have all the tantrums you want in your mind,” one of my doctor friends said with a slightly irritable undertone. “But in front of your staff and patients, you’ve got to keep it together.”
This attitude of resilience results, at least in part, from the harsh training these doctors experienced in medical schools. Brutal shifts, sometimes 48 hours or longer, along with relentless browbeating by superiors, can condition doctors to show no weakness, to simply “suck it up” and act as if nothing is wrong.
Whether it’s due to temperament or training, this attitude leaves an imprint on how physicians deal with their own health. In Germany, only 20 percent of all physicians have their own family doctor. In the United States, it’s 40 percent. In both Europe and America, doctors are the one professional group that takes the least sick days.
The decision to work while ill is primarily based on practical considerations. Many hospitals are understaffed, and a doctor on sick leave puts an additional burden on his colleagues.
For a doctor in private practice, like a surgeon who operates in an outpatient facility, falling ill on short notice entails a series of major organizational and financial ramifications: Patients have made arrangements for the day of the procedure, from fasting to setting up a ride. The operating room has been booked, along with a staff of anesthesiologists and surgical nurses.
In order to avoid embarrassment, hassle and inconvenience, some sick doctors load up on whatever drugs are needed to mask the symptoms and to help them power through the day, hoping they won’t make a mistake that can put their patients and, subsequently, their own careers at risk.
Another response to the mounting pressures is withdrawal. After seeing patient after patient all day long, another physician friend told me that she just doesn’t feel like talking anymore, not with friends, not with relatives, sometimes not even with her own husband and kids. “I guess I’ve become kind of an introvert,” she said.
My friend has found ways to recover, and her family life is still intact. For many physicians though, that is not the case. Divorce, family troubles and social isolation are on the rise in the medical community.
Some doctors seem to develop an outright disgust for certain patients – their attitude of entitlement, their runaway expectations, and their disrespect for the physician’s time. A surgeon I recently spoke with told me that the day when he does surgery has become the highlight of his work week. That’s not just because he enjoys performing procedures, working with his hands, as surgeons do, but more importantly because the patients are sedated and therefore quiet.
Some of this is purely anecdotal, of course. But the legal, political, and economic environments in which doctors practice medicine these days, not just in America but in the entire industrialized world, is like walking on a high wire without a safety net. And up there, in thin air, the specter of the disruptive doctor can materialize at any second.
Katja Ridderbusch is an Atlanta-based foreign correspondent for German news media, including the national dailies “Die Welt” and “Der Tagesspiegel,” as well as German national public radio. She frequently reports about health care in the United States.