Georgia improved on several important health measures from 2007 to 2012, but its overall health care ranking among states fell from 35th to 45th in a newly released study.
The Commonwealth Fund’s 2014 state health system scorecard, released Wednesday, found that all states saw meaningful improvement on at least seven of 34 indicators.
Georgia improved on 13, including child vaccinations, hospital admissions for pediatric asthma, Medicare 30-day readmission rates, and infant mortality.
But Georgia’s health statistics worsened in 12 areas, including its rates of uninsured adults; adults with a usual source of care; and adults without a dental visit in the past year.
Overall, states made little progress in improving health care access, quality, and outcomes and lowering costs in the five years preceding implementation of the major provisions of the Affordable Care Act, the Commonwealth Fund report’s authors said.
The study could be used as a baseline to test whether the ACA has a substantial effect on health care.
Bill Custer, a health insurance expert at Georgia State University, said the findings reflect the impact of the recession on access to health care.
“The recession hit health care here harder than other places,’’ said Custer, adding that many Georgians lost health insurance and access to medical care as their personal income plunged.
Georgia started with higher levels of chronic illness, and those medical outcomes are affected by poor access to medical care, he said.
The state ranked 44th in adults who went without care because of cost in the past year.
“This study shows the health effects of the recession and lost coverage,’’ Custer said. “It indicates how vulnerable that Georgia is.”
Among the national findings:
** Thirty states saw a decrease in the rate of older adults receiving recommended preventive care, such as screening for cancer. (Georgia had no change in this area.)
** Nationally, fewer seniors with Medicare coverage were prescribed high-risk medications, including in Georgia.
** Medicare hospital 30-day readmission rates declined in a majority of states, but rates vary widely. (The re-hospitalization of a recently discharged patient is costly and may indicate problems with care.)
** Mortality measures improved in many states, as 44 had lower colon cancer death rates, including Georgia, and 35 had lower breast cancer death rates (Georgia had no change on this measure).
** Preventable deaths rates varied widely: Twenty-five states, including Georgia, improved on a key mortality measure—deaths before age 75 from conditions that could have been treated through early detection and high-quality care.
** Rates of premature death remained higher among blacks than among whites in all states, although the gap did narrow nationally during the periods 2004–05 and 2009-10.
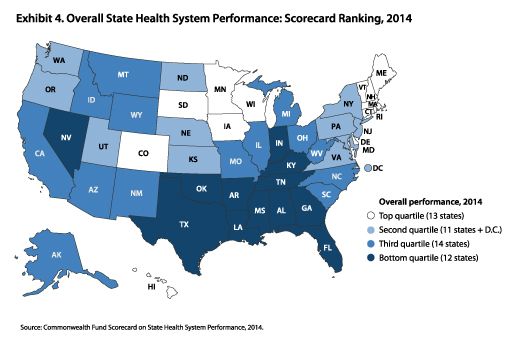
The top-ranked states are Minnesota, Massachusetts, New Hampshire, Vermont and Hawaii.
Southern states generally performed in the bottom quartile on health measures, with exceptions including South Carolina, North Carolina and Virginia. (Here’s a GHN article on Kaiser Family Foundation’s report on the Southern states’ health challenges.)
The Commonwealth Fund estimated the impact for each state if it reached the level of the best-performing state. But Cathy Schoen, co-author of the report, added that for people in low-ranking states, “even reaching average would make an enormous difference.”
“In the United States, where you live has long determined the kind of health care you receive, and it shouldn’t,” Dr. David Blumenthal, president of Commonwealth Fund, said in a statement. “The Affordable Care Act has the potential to level the playing field, as all states have the opportunity to make substantial improvements to their health care systems if they take full advantage of the law, including Medicaid expansion.”