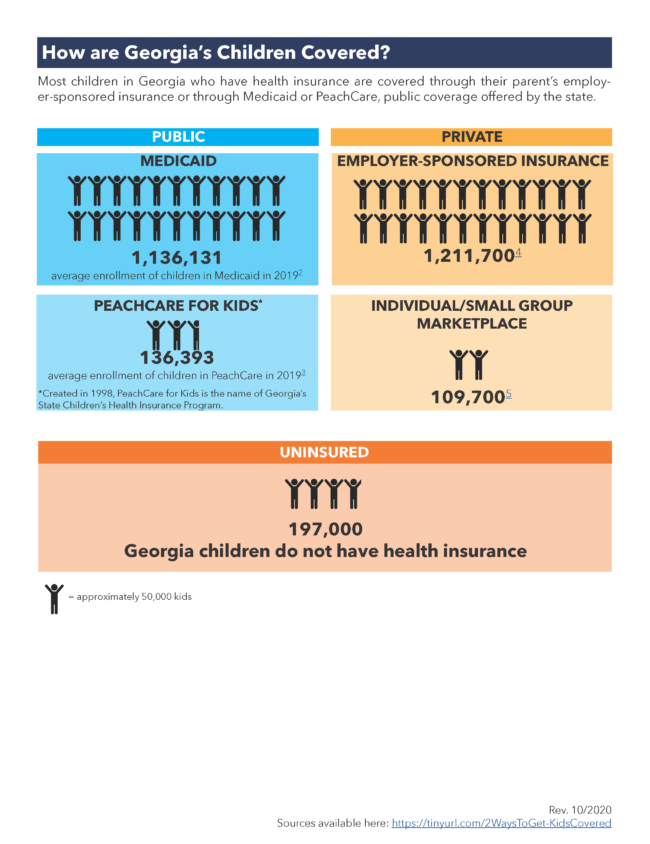
Tens of thousands of uninsured Georgia children could gain a pathway to health coverage under a House bill moving through the General Assembly.
The legislation, if approved, would lead to the state creating “express lane eligibility’’ for many kids receiving food stamps to be automatically added to the Medicaid program.

About 7 percent of children in Georgia are uninsured, a higher percentage than the national average. A majority of kids eligible for food stamps are also eligible for Medicaid because of their family income level, but many are not enrolled in the government health program.
House Bill 163, which passed the House Health and Human Services Committee earlier this week, would direct the Georgia Department of Community Health to submit the new enrollment mechanism to federal officials for approval.
Other states, including Alabama, South Carolina and Louisiana, have already adopted the express lane – and have increased coverage of uninsured children, said the bill’s lead sponsor, Rep. Sharon Cooper, a Marietta Republican who’s chairman of the health committee.
“This is especially important for people in rural areas’’ because they often lack broadband or cellphone service, or transportation to a DFCS office, Cooper said. “We are delaying children from getting health care when they are eligible to have it,’’ she told her committee Tuesday.
Supporters of the legislation point out that the bill would not create a new eligibility category.
Medicaid, jointly financed by the states and federal government, covers low-income and disabled people, including about 2 million in Georgia. Medicaid enrollment in the state has surged during the pandemic – including thousands of children — but experts believe that a large number of Georgia families still lack health insurance coverage due to the COVID-19 crisis.
The express lane can save the state money on processing separate applications, said Tom Rawlings, head of the state’s Department of Family and Children Services, which handles enrollment for both SNAP (food stamps) and Medicaid.
It costs Georgia $35 a case to add a child in one program to another, Rawlings said. The eligibility move, if approved, “saves a lot of time and expense.’’

It can also increase early preventive care for kids, he added, and keep them from needing hospitalization or state services such as foster care. Many children come under state supervision “because they’re not getting the medical or behavioral health care they need.’’
Children’s advocacy groups, medical provider groups, state officials and others have enthusiastically supported the change, which they say could lead to up to 70,000 uninsured children in Georgia getting health coverage.
“With nearly 200,000 children lacking health insurance, state eligibility workers putting in long hours and health care providers struggling to keep up, we are excited that this policy can help address all three of these challenges at once,’’ said Erica Fener Sitkoff of Voices for Georgia’s Children, an advocacy group that brought the idea to Cooper. “Most important, it will make it easier for struggling families to both feed their children and not worry about whether or not they can afford to take care of their children’s health needs.’’
Rep. Jesse Petrea, a Savannah Republican and member of the House panel, said, “We don’t need barriers in any way, shape or form to getting children the care that they need.’’
Studies show kids who get Medicaid go farther in school and are healthier and more successful financially as adults compared to those who have no insurance or inconsistent coverage, Laura Colbert of the advocacy group Georgians for a Healthy Future told the House panel.
After creating the express lane, Alabama now has an uninsured rate of just 3.5 percent, said Callan Wells of the Georgia Early Education Alliance for Ready Students.
“Surely we can do better” than that in Georgia, Cooper replied.