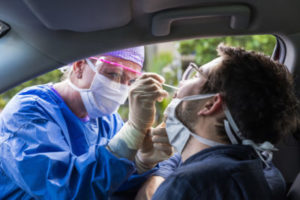
New COVID-19 cases in Georgia jumped by more than 4,500 on Tuesday, the highest daily increase reported in months.
Most of the new cases came from rapid antigen tests. About 1,000 of those positives, though, were part of a “data dump’’ of cases from October, state officials said.
How the rapid antigen tests are counted has generated questions and confusion in Georgia. The antigen test results are now posted separately on the Georgia Department of Public Health’s daily COVID report, but those positives aren’t included in data the state sends to external agencies as confirmed cases.

“We’re really not painting an accurate picture of what’s going on,’’ Amber Schmidtke, a microbiologist who tracks COVID in Georgia in the Daily Digest, said Wednesday.
Other Southeastern states report the rapid test results as part of their cumulative infection totals, she said.
She called the Tuesday infection increase in Georgia ‘‘a little frightening.’’ The test positivity rate here has also increased, she said.
Wednesday’s COVID numbers reported by the state declined from the Tuesday total to 2,350, but with a high number of confirmed deaths — 69.
The antigen testing numbers “fluctuate widely one day to the next,’’ said Nancy Nydam, a Public Health spokeswoman. Those fluctuations will smooth out more as medical facilities get used to reporting these results, she added.
Rapid tests are not considered as accurate as PCR tests. But because they are faster and less expensive than PCR tests, antigen tests may be more practical to use for large numbers of people, experts say. They’re frequently used at universities, long-term care facilities and medical offices.
There’s an increased chance of a false negative result with an antigen test, meaning it’s possible to be infected with the virus even though the test indicates you are not. But a positive result on an antigen test — indicating that you are infected — is considered accurate when instructions are carefully followed, the Mayo Clinic says.
If a person has COVID symptoms and gets a negative antigen test, they may want to follow it with a PCR test, experts say.
National figures are troubling
The overall rise in new infections in Georgia coincides with an alarming national increase in COVID cases.
The stunning numbers were somewhat overshadowed this week when Pfizer announced Monday that early clinical trial data suggested its coronavirus vaccine was more than 90 percent effective.
Still, at least 1,448 new coronavirus deaths and 139,855 new cases were reported Tuesday in the United States. And COVID-19 hospitalizations hit a record high of 61,964 the same day. The number of Americans hospitalized due to COVID-19 has risen almost 50 percent in the last two weeks.
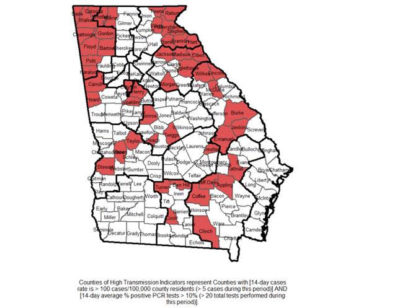
Georgia is categorized as a state with “uncontrollable spread’’ by covidexitstrategy.com. The website reports that the state is meeting just 41 percent of its testing target.
And the recently released White House Coronavirus Task Force report said Georgia was in the “red zone’’ for major community spread of the disease. It joined 42 other states in this category.
The report said hard-hit counties in the state must take a proactive approach, testing all people in the 18-to-40 age group whether or not there are any other risk factors. “Georgia must expand the mitigation efforts statewide as test positivity and cases are increasing,’’ the task force said.
It added that during the week of Oct 26 – Nov 1, 10 percent of nursing homes in Georgia had at least one new resident infected with the virus; 19 percent had at least one new staff COVID-19 case, and 4 percent had at least one new resident COVID-19 death.
“We have been experiencing a significant surge for the past five weeks, as reflected in rising case counts and positivity rates and are now also seeing increases in both hospitalizations and deaths,’’ said Dr. Harry Heiman, a public health expert at Georgia State University. “Tragically, this is in line with what is happening all over the country and in our state.
“Like many other places, there has been a failure of political and public health leaders to take meaningful action,’’ Heiman said. “We know a mask mandate works, we know that allowing large in-person gatherings, including political events, adds to transmission.’’
State public health officials should also focus on the disproportionate impact of COVID on communities of color, Heiman added.
“I am hopeful that a new [presidential] administration will provide not only a coordinated national framework and plan, but also provide states with the resources they need to be successful.’’
Outbreaks at schools in Richmond, Peach and DeKalb counties have shut down classrooms this week.
Stronger guidance on masks
The CDC, in a major update to its guidance, said Tuesday that a mask protects the person who wears it, and not just people near the wearer. The Atlanta-based agency also noted that numerous studies have demonstrated the benefits of “universal masking policies.”

Meanwhile, the supply of personal protective equipment – a big concern early in the pandemic – is again leading to worry about shortages as colder months approach, raising the potential for big caseloads of COVID and flu patients.
The Strategic National Stockpile, the nation’s emergency reserve, has only 115 million N95 masks, far short of the 300 million the federal government had hoped to amass by winter, Rear Adm. John Polowczyk, who retired on Monday as the national supply chain commander, said in a recent interview, according to the New York Times.
Governors are once again competing with one another and with big hospital chains for scarce gear, the Times reported.
WABE noted that as Thanksgiving approaches, the U.S. is regularly breaking records for new COVID-19 diagnoses.
“Now you have a holiday where it’s colder, people are more likely to be inside celebrating with family, likely to have more travel as well as case counts are much higher,” said Cria Perrine, an epidemiologist with the CDC, the WABE article reported. “This has got the potential to be sort of the perfect storm.”