Brenda Ulmer, a longtime operating room nurse, was walking to her car after one of her shifts when she suddenly realized she didn’t feel well.
“My chest felt tight, my throat hurt, my nose was burning,” recalls Ulmer, who lives in the Atlanta suburb of Snellville. She was feeling sick to her stomach, too. “I remember distinctly thinking that I must be getting the flu,” she says, so she went straight home.
Unfortunately, that was not the end of the problem. “That sick feeling happened again about a month later,” she says. “I had worked full 8-hour operating room shifts both times.”
Ulmer eventually received her diagnosis: late-onset asthma. The disease will be with her for the rest of her life.
She attributes her problem to “surgical smoke,’’ something that many non-medical people have never heard of.

Where does the smoke come from? It’s produced in the operating room as lasers and electrosurgical devices cauterize or vaporize human tissue.
Just like cigarette smoke, the smoke generated by surgery can be seen and smelled. Worse than that, it can affect a person’s health.
Dustin Cain, president of the Georgia Assembly of Surgical Technologists, says, “The average daily impact of surgical smoke to the OR team is equivalent to smoking 27 to 30 unfiltered cigarettes.”
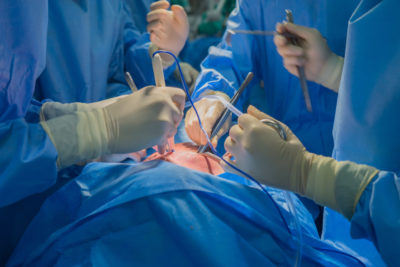
This situation is especially bad for operating room nurses, whose shifts often last 8 to 12 hours. While surgeons may work on one or two patients within that span of time, nurses may stay in the OR much longer, assisting one surgeon after another, rotating from one procedure to the next.
Surgical smoke would be a nuisance even if it were harmless, because it has a repulsive odor. But studies show it contains toxic gases; vapors and particulates; viable and non-viable cellular material; as well as viruses and bacteria.
An estimated 500,000 health care workers are exposed to surgical smoke each year, according to the Occupational Safety and Health Administration. Exposure to these substances can cause short- and long-term health problems, such as eye, nose and throat irritation, and possible long-term illnesses, such as emphysema, asthma and chronic bronchitis.
Bill meets resistance
Georgia Senate Bill 347, sponsored by Sen. Gloria Butler (D–Stone Mountain), would require hospitals in the state to install surgical smoke evacuation equipment in all surgery rooms, both in hospitals and surgery centers.

Two states, Rhode Island and Colorado, already have such laws, and some other states are considering them, nurses say.
The Senate Health and Human Services Committee heard testimony on the bill earlier this month at the state Capitol, but did not take a vote.
Opponents of the legislation questioned the efficacy and cost of existing smoke evacuation systems, which some hospitals already use.
Anna Adams, a lobbyist for the Georgia Hospital Association, said at the hearing that the legislation would impose an unfunded mandate on hospitals.
Tim Kibler, of the Georgia Alliance of Community Hospitals, said some surgeons complain that the smoke evacuators “impair their ability to perform the surgery.’’
Dr. Joe Sharma, of the Department of Surgery at Emory University School of Medicine, testified that ‘’the smoke generated from using thermal cautery or ultrasonic energy or laser can potentially have risks. And I agree with that potential,” he said.
But Sharma questioned the effectiveness of the evacuation systems, and the data surrounding their use.

Proponents of the legislation include OR nurses and surgical techs.
Many Georgia hospitals have the equipment to reduce the amount of smoke the operating room staff is exposed to, says Vangie Dennis of Atlanta, a longtime operating room nurse.
A January study in JAMA Surgery, though, states that only 14 percent of operating room workers surveyed always used smoke evacuators. Factors contributing to the non-use include exhaust noise, obstruction of the operating space, and a lack of awareness of surgical smoke hazards.
A sensitive issue for nurses
Still, Northside Hospital began an initiative about three years ago to make all its operating rooms smoke-free, according to Katherine Watson, spokeswoman for the Atlanta-based system.
“We began by increasing awareness of the hazards of surgical smoke and providing education to our physicians and staff through continuing education opportunities,’’ she says. “Several Northside doctors championed our initiative.”

“Small-particulate matter that is found in the surgical smoke is easily inhaled and can cause numerous health problems,” says Dr. Guilherme Cantuaria, a Northside Hospital gynecologic cancer surgeon.
“Numerous articles have stated that daily inhaled surgical smoke could be equivalent to smoking dozens of cigarettes,” Cantuaria says.
Pat Thornton, who attended the hearing, noted that she has been an operating room nurse for more than four decades. “Smoke has always been an issue for me,” she said. “It has affected me personally with sinus infections, nosebleeds and laryngitis about three or four times a year.”
Thornton, who lives in Palmetto, south of Atlanta, agrees with Ulmer that surgical smoke has a cumulative effect. And the effect can be felt during a single long shift.
When an OR nurse works a surgery like a double mastectomy, it takes its toll, says Thornton. “The smoke from that type of surgery will make me completely hoarse before leaving the hospital,” she said.
Legislative action on surgical smoke doesn’t look likely this year. There has been no vote on Sen. Butler’s proposal, and Thursday is the deadline for bills to pass at least one chamber of the General Assembly or be considered dead for the 2020 session.
Butler, though, said she is glad she started the conversation about surgical smoke. She has requested a legislative study committee on the issue.
OR nurse Dennis says, “Even if surgeons are not convinced, more times than not they will use certain devices as along as it does not interfere with surgery and they [the surgeons] are included with the hospital’s decisions,” she says.
“We work in this environment by choice and for the health and safety of our patients. That’s what this bill is about.’’
Judi Kanne, a registered nurse and freelance writer, combines her nursing and journalism backgrounds to write about public health. She lives in Atlanta.

