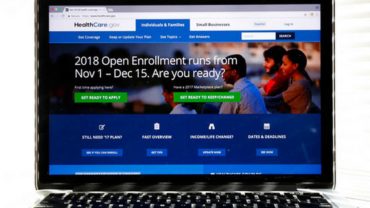
All of the political campaign talk on health care may have obscured the reality that starting Thursday, the health insurance exchange opens for business.
Open enrollment for Georgia’s 2019 exchange, which operates under the Affordable Care Act, runs from Nov. 1 to Dec. 15.
The coverage rules will feature a significant change: People who previously faced a tax penalty for not having health insurance will no longer be penalized in 2019. (Congress repealed the ACA’s health insurance requirement.)
And for some Georgians returning to the exchange, there may be good news on prices. Two of the four health insurers are set to make reductions in monthly premiums from the rates they offer this year.
Such easing of prices, coming on the heels of a year of increases of more than 50 percent, has added more stability to the exchanges in states around the country. The ACA created them for people without job-based or government insurance.
Another big change for this enrollment period is the drastic cut in funding for the insurance counselors known as navigators, both in Georgia and nationally. The total navigator funding for Georgia’s 2019 enrollment period, $499,995, is about one-third of the funding for the 2018 sign-ups in Georgia.
Georgia Refugee Health and Mental Health, a nonprofit based in Clarkston, will get the state’s entire navigator funding.
Bill Custer, a health insurance expert at Georgia State University, said Wednesday that the cut in navigator funding may hurt rural areas that don’t have Internet access. Sign-ups are executed through the website healthcare.gov.
“It certainly will impact people who are less connected and who don’t have the resources to research their choices,’’ he said.
Those with pre-existing conditions want to have their choice of doctors and prescription drugs for their health challenges, Custer added. Without help from navigators, they may have more difficulty making the correct choice of health plans for their medical needs.
The federal Centers for Medicare and Medicaid Services, when it announced the navigator funding reductions, said using insurance brokers and agents is more economical. It also said in a statement that the exchanges have become more familiar to Americans seeking health insurance, somewhat reducing the need for federally funded navigators.
About 480,000 people bought coverage this year through Georgia’s exchange, which like most state exchanges is run by the federal government.
The individual mandate, the official name for the former requirement to have health insurance, was unpopular with many consumers, which led to its repeal. But it was originally put into the ACA to encourage widespread health coverage. Some observers have expressed concern that without it, many more people will take the risk of going uninsured.
Custer, however, said the disappearance of the rule may not affect exchange enrollment that much. “The mandate was weak in terms of penalties and enforcement,’’ he said.
Kathleen Connors, head of Georgia Refugee Health and Mental Health, said Wednesday that “there is a great deal of uncertainty” among the general public about whether the ACA survived the Republican attempts to repeal it, and about the individual mandate. She also said that the flattening of premiums, and insurers expanding geographic coverage in Georgia, have added stability to the exchanges.

“It’s a more competitive environment in terms of choices for people,” Connors said.
She said her organization has established a call center (1-888-230-7772), hired navigators, contacted media, and is working with health care systems and medical providers in getting the word out on enrollment.
Kaiser Health News, meanwhile, reported that in the span of less than 12 hours last week, the Trump administration took two seemingly contradictory actions that could have profound effects on exchanges.
First, officials issued guidance on a new approach that makes it easier for states to get around some ACA requirements, including allowing the use of federal subsidies for skimpier plans that can reject people with pre-existing conditions, KHN reported.
Yet the other move — a proposed rule unveiled Monday evening — could bolster ACA marketplaces by sending millions of people with job-based coverage there, armed with tax-free money from their employers to buy individual plans.
The administration and Republicans in Congress say they are looking to assist those left behind by the ACA — people who don’t get subsidies to help them buy coverage and are desperate for less expensive options — even if that means purchasing less robust coverage, Kaiser Health News reported.

In August, the administration released a rule allowing expanded use of short-term plans, which are less expensive than ACA policies. To get those lower prices, most of these plans do not cover prescription drugs, maternity care, mental health or substance abuse treatments.
Under the rule, insurers can sell them starting in 2019 for up to a year’s duration , with an option to renew for up to three years, reversing an Obama-era directive that limited them to 90 days.
Under the new guidance giving states more flexibility on what is offered, consumers could again see a wide variation on coverage, premium rules and even subsidy eligibility.
A proposed rule also allows employers to fund tax-free accounts — called health reimbursement arrangements (HRAs) — that workers can use to buy their own coverage through the ACA marketplaces.
The administration estimates about 10 million people would do so by 2028 — a substantial boost for those exchanges, according to Kaiser Health News.