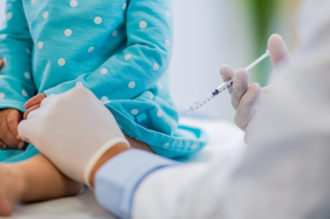
This flu season in Georgia and the South is shaping up to be harsher than the last one.
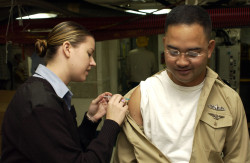
Georgia is one of seven states overall — most of them in the Southeast — that have reported “widespread’’ flu activity, according to a new CDC report, tracking the week ending Dec. 2.
“Flu is increasing. We’re seeing a pretty steep increase in influenza activity across the U.S. but especially in the South,” Brendan Flannery, a co-author of the new report and an epidemiologist in the CDC’s flu division, told CNN.
The Georgia Department of Public Health said Friday that there have been 47 influenza-associated hospitalizations in the eight-county metro Atlanta area so far this season. This time last year, there had been 26 such hospitalizations, the agency said.
No flu-related deaths have been reported in Georgia.
Arkansas, Louisiana, Massachusetts, Mississippi, Oklahoma and Virginia also reported widespread activity.

Public health officials urge that everyone 6 months and older get a flu shot. The CDC, though, reports that fewer than half of Americans have received the vaccine so far this season.
Concern about a severe flu season comes from several factors, including signs that the season started a few weeks earlier than usual, NPR reported.
“When you have an early start with regional outbreaks, that is generally not a good sign,” said Anthony Fauci, who directs the National Institute of Allergy and Infectious Diseases. “Sometimes that’s the forerunner of a serious season.”
An early start could mean a longer season, which could mean more people end up getting infected with the flu, according to the NPR article.
Another reason for concern is that Australia had a severe flu season this year. (Because that country is in the Southern Hemisphere, its fall-winter flu season occurs during our spring and summer months.)
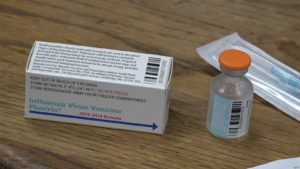
A major reason for Australia’s problem is that the main strain of flu circulating there was one known as H3N2. That kind of flu virus tends to make people sicker than do other strains, especially the elderly, NPR said.
To make things worse, the flu vaccine appears to have been only about 10 percent effective against that strain in Australia. Part of the reason for that is that flu strains are constantly changing and the H3N2 strain used to make the vaccine mutated during production of the vaccine. This weakened the shot’s effectiveness.
“The mutation just happened to be in a very bad spot on the virus to make it essentially be a mismatch for the vaccine,” Fauci said.
The United States is using the same vaccine, and an H3N2 strain appears to be dominating outbreaks in this country so far. But it could also turn out that the vaccine could be far more effective in the United States than it was in Australia, according to Flannery of the CDC.
That’s because a slightly different H3N2 strain could end up dominating in this country, for example. Another possibility is that other flu strains could become more common. The vaccine provides stronger protection against those.
Dr. William Schaffner, an infectious disease specialist at Vanderbilt University, told CNN that “vaccine effectiveness” is not the sole measure of a vaccine’s benefits.
“When we measure vaccine effectiveness, that’s . . . protecting against disease completely,” said Schaffner.
“What’s not measured is that, even if you get the flu in spite of the vaccine, your flu case is likely to be milder; you’re less likely to have the complications of pneumonia, having to be hospitalized and dying,” he said.