This article was jointly reported by WebMD Health News and Georgia Health News
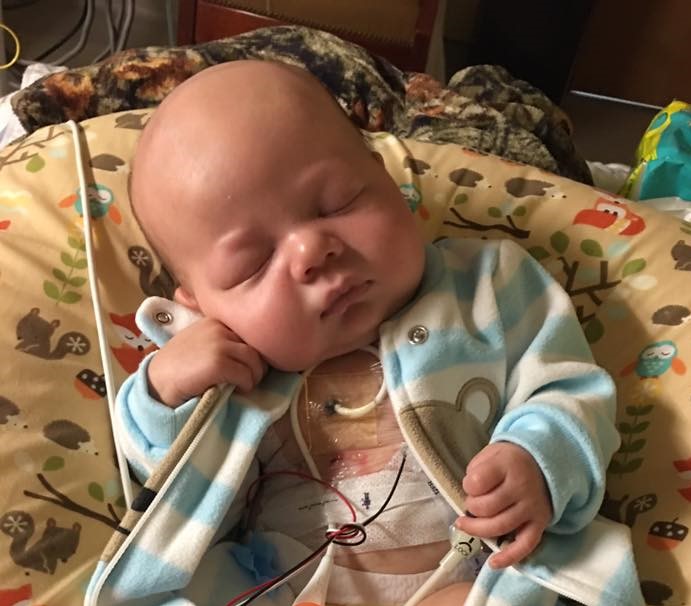
Jackson Garcia was born “healthy and round and full of hair.”
But at 5 months old, he started getting fussy around mealtimes and refused food. “My worst fear was colic,” said his mother, April Garcia, who lives in Lawrenceville, Ga..

When Jackson didn’t improve, he was admitted to the hospital. After a few days of keeping him in intensive care, his medical team called the Garcias into a room filled with doctors.
“We know what’s wrong with Jackson,” they said.
It was a death sentence called Krabbe disease.
In Krabbe (pronounced crab-ay), the body fails to produce enough of an enzyme that’s key to wrapping protective insulation called myelin around nerves. Without it, the brain and nerves deteriorate. Children who develop symptoms as babies become irritable and hard to soothe around 6 months, and they lose their ability to swallow. Their muscles start to spasm and contract. That’s followed by mental deterioration, blindness, deafness, and seizures.
Babies with Krabbe typically die before their second birthday, and it is an agonizing death.
The doctors told Garcia they were sorry. Nothing could be done. There was a treatment, but it wouldn’t help Jackson. His disease was already too advanced.
Garcia didn’t believe them. She got onto the computer. She searched for any hope.
“You know what the advice [on the Internet] is?” she said. “Go home and take pictures, so we have pictures.”
Garcia told Jackson’s story as she recently testified before the Georgia House Health and Human Services Committee in support of a bill that’s been named Cove’s Law, for 19-month-old Cove Ellis, another child in Georgia recently diagnosed with Krabbe disease.
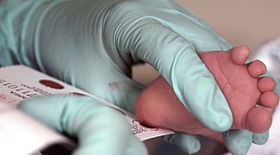
The bill they are asking the Legislature to pass, House Bill 241, would give parents in Georgia the option to have newborns screened for Krabbe. The bill cleared the state House of Representatives last week and now heads to the Senate for consideration. The screening would cost $5 to $7 per test, which involves taking a small spot of blood from an infant’s heel.
Many doctors and geneticists have doubts about the screening, however. While they are sympathetic to the parents’ cause, they say it will do more harm than good.
Krabbe has no cure. There is a treatment available — a stem cell transplant — but it’s very risky. Not all children survive it. Those that do often face physical and developmental delays. The treatment can cause other problems, too, including damage to the heart, lungs, or liver and a severe complication called graft-versus-host disease — where the transplanted cells attack their host body, causing problems like organ damage, joint pain, and fatigue that can last a lifetime.

Then there are problems with the screening test. One is that it has a high percentage of false positives. One recent study found the test correctly identifies a child who has the early, aggressive form of the disease about 1 percent of the time.
The other 99 percent of children who test positive won’t have the disease, but they’ll still need additional tests to rule it out. Those additional tests can produce their own uncertain results that can leave many families in a kind of medical limbo. These families go through a different kind of torment, one that’s not often heard about by the state legislators.
“Everyone wants to do the right thing for kids,” says William Wilcox, MD, PhD, a professor of human genetics at the Emory University School of Medicine. The testing, he said, “is being pushed with the wrong information. They’re doing real harm. When there is better testing and treatment, we will support screening for all babies.’’
Garcia says she’s aware of the debate over screening and the latest science. She keeps up with families who’ve benefited from the stem cell transplants and feels like others should at least have the chance to make a choice she did not. Her son, Jackson, died in October.
“I promise I’m not just living in a fantasy world,’’ Garcia says.
A harsh treatment offers hope
The form of Krabbe disease that strikes newborns is caused by a change, or mutation, in the gene that carries the blueprints for an enzyme called galactosylceramidase, or GALC for short. The disease is rare, striking between 1 in 100,000 and 1 in 350,000 babies.
Before doctors figured out how to screen newborns for Krabbe, the way most parents discovered they carried the gene was that they watched a child die from it.

A 2005 study published in The New England Journal of Medicine was the first sign of hope for these families.
In that study, researchers at Duke University and the University of North Carolina described the outcomes of pioneering stem cell transplants for babies who had been diagnosed with Krabbe. The stem cells are derived from donated umbilical cord blood.
Study author Joanne Kurtzberg, MD, who pioneered the transplants and is director of Duke’s pediatric bone marrow transplant program, says the donor cells can help replace the missing enzyme.
To prepare for a transplant, doctors give babies powerful chemotherapy drugs that kill their diseased cells and suppress their immune systems. This takes 10 days.
After the chemotherapy, the babies get the donated stem cells through an IV. If all goes well, the cells travel to the bone marrow and begin to grow, replacing diseased blood cells with new cells that can produce the missing enzyme. Of the 25 children enrolled in the original study, 11 were newborns who had not yet begun to show symptoms of the disease, and 14 were older babies who had already begun to deteriorate.
Eight of the 14 older babies died during or shortly after their transplants. The rest of those children did not die, but they also didn’t really improve, Kurtzberg says.
But for the 11 youngest babies, the results were astonishing. At the time the study was published, researchers had followed them for three years. They were all still living. Six had already had longer lives than their siblings who had died of Krabbe.
Aware of the promising results, former Buffalo Bills quarterback Jim Kelly and his wife, Jill, persuaded lawmakers in New York state to start screening babies for Krabbe, which had afflicted their son Hunter.
The Kellys run a foundation called Hunter’s Hope that supports families affected by Krabbe and lobbies for newborn screening.

New York launched its program in 2006, and three other states — Missouri, Kentucky and Ohio — have also added Krabbe to their newborn testing panels.
But momentum has slowed as other evidence surfaced about the ambiguities of testing and the value of the treatment. Six other states — Illinois, Louisiana, New Jersey, New Mexico, Pennsylvania and Tennessee — have passed laws that would allow screening but have not yet implemented their programs. In some of those cases, state health departments have blocked screening for Krabbe, citing both the expense of the testing and the lack of clear benefit from the treatment.
Many of these states point to a decision issued by the Secretary’s Advisory Committee on Heritable Disorders in Newborns and Children, a national panel that makes recommendations for newborn screening for the U.S. Department of Health and Human Services. In 2010, the panel reviewed the evidence for screening children for Krabbe. It concluded that the disease should not be added to a recommended list of 32 disease screenings that scientists say clearly benefit children.
The panel found that while infants with the early onset form of the disease probably would benefit from early detection, they also found “substantial harm is possible (either from testing and/or identification; from treatment/other interventions, or both).”
Hard lessons learned in New York
Researchers who reviewed results from New York’s program agreed. From 2006 through 2014, the state screened almost 2 million infants by pricking their heel and swabbing a small spot of blood on a card.
Of those tests, nearly 350 families got a call that their baby might have Krabbe.
Of those 350 families, additional testing confirmed the early, aggressive form of Krabbe in just five babies, making the disease much rarer than doctors initially thought. Two other babies were identified as at risk for the disease but didn’t have a definite diagnosis.
Doctors offered the risky stem cell transplants to seven of the families.
Of the five with confirmed Krabbe, one family declined the transplant, and their baby died at 18 months. Of the four babies who went through with the procedure, two died of complications of the transplant. The other two have survived, though with some challenges.
The first survivor, who was 8 at the time the study was published, needs help to walk, and his growth has been stunted, though he can understand what people say to him. The other child, 5 at the time, had developed graft-versus-host disease, and doctors in New York say she is failing to thrive.
In the two kids where the diagnosis was iffy, parents refused the transplant but did agree to let doctors follow their children with additional testing. Over time, those babies improved, and they were no longer considered candidates for transplant. Researchers consider those cases to be uncomfortably close calls, given the risks of the transplant itself.
Bobbie Salveson, a nurse practitioner, was studying for her PhD as New York began screening for Krabbe. She became involved with the Krabbe families because her mentor was helping to implement the program. She eventually focused her graduate work on the project.
“I’ve been a nurse and a nurse practitioner for more than 30 years. I’ve seen a lot. That was probably the worst disease I’ve ever seen. It’s truly horrific,” says Salveson, who is now a clinical assistant professor of at the University of Washington in Seattle.
“But, the kids who got transplanted didn’t do a whole lot better. Better, I guess, in that they weren’t arched back and screaming all the time; but better as far as development, not so much,” she says.
Salveson also reached out to families who initially got a call that their baby might have Krabbe but were later cleared of the disease. Many of those families declined to participate in her research. They wanted to put their brush with Krabbe behind them, but a few agreed to share their stories.
One mother told Salveson she had so much anxiety after the screening that doctors prescribed her “pills for depression and stuff like that.” Later, she started hurting herself. “It was a way to get the pain off me, I guess, even though the pills weren’t helping,” she told Salveson.
Another mother said the shock of the test results caused her breast milk to dry up. She was never able to breastfeed her daughter. “I was pretty sick. I couldn’t eat. I thought she was going to die,” she said.
Specialists who saw the babies deemed to be at high risk told Salveson that many families who initially got positive test results were furious. They had never consented to the screening. They wanted to know why their babies who seemed perfectly healthy were now going through invasive follow-up tests like spinal taps only to get uncertain results.
In 46 cases, the kids didn’t have the early onset form of the disease, but gene tests and imaging scans suggested they could get it later, though doctors couldn’t tell their parents when that might happen or how to live with such an uncertain prognosis.

After eight years of screening, it turned out that the Krabbe screening test used in New York correctly detects a baby with the early aggressive form of the disease only about 1 percent of the time.
“There were two lives that were saved because of it. I wish the treatment was more effective in terms of them having fewer delays and better growth than they’re having,” says study author Melissa Wasserstein, MD, chief of the division of pediatric and adolescent medicine at Children’s Hospital at Montefiore in New York.
“It is concerning that we’re just kind of transforming it into more of a chronic disease,” she says.
The results of the New York screening program were published in December in the journal Genetics in Medicine. In a commentary on the study, an independent expert says the outcomes suggest that New York should put its newborn screening program for Krabbe on hold, until either the screening test or the treatment improves.
In an emailed statement, the New York Department of Health says that it is trying to refine its screening program for Krabbe but that it continues to test infants for the disease.
“The evidence shows that Krabbe screening has cost the state a lot, both in dollars for the testing itself, in physician time to examine children who have a screening test that turns out to be a false positive, in parental anguish among the children who are thought to be at risk but, to date, have no symptoms of disease. Clearly, after over 2,000,000 screening tests, the program has yet to show any of the benefits that people were hoping it would,” says John Lantos, MD, director of pediatric bioethics at the University of Missouri-Kansas City School of Medicine.
Reconciling the evidence
Screening advocates disagree that the New York program was a failure.
“The outcome for children who aren’t diagnosed in time for treatment versus those who are is tremendous. I’ve met several children who have undergone treatment — they go to school, they’re mobile, they’re able to communicate, and most importantly, they are living,” says Anna Grantham, a spokeswoman for Hunter’s Hope, in a written statement to WebMD.

Kurtzberg, the doctor who leads the stem cell transplants at Duke, has not published a long-term follow-up study on the 50 children with Krabbe that she’s transplanted since 1995.
But she says they basically fall into three different groups. The first group is “pretty normal.” The second group can think and reason, and they have pretty good upper body function — they can talk and eat, but they need some help walking. The third group requires wheelchairs, and they “look like kids who have cerebral palsy.”
In an email, Dr. Kurtzberg said the oldest living survivor from her program is now 22.
She says she’s learned that the transplants work best when performed before babies are 30 days old, which makes finding these kids a race against time. That’s the main reason she says she’s a strong advocate for screening.
Other researchers question the long-term outcomes of babies given stem cell transplants for Krabbe, including the babies transplanted at Duke. The last time experts shared results publicly was at a meeting in 2008 in Holiday Valley, NY.
Of the 16 babies originally transplanted at Duke before they showed symptoms, all were spastic, meaning they had trouble controlling their muscles; five had tubes implanted in their stomachs to help with feeding; and all had delayed growth. They were able to understand speech, but all had trouble speaking themselves. Half needed braces or canes to walk, while four were able to walk on their own. Doctors had judged their brains and mental functions to be normal.
“Dr. Kurtzberg’s conclusions are incomplete,” Salveson says. “I would feel far better about this if there was a quality-of-life study done, but there hasn’t been; or if they were able to actually speak to the parents who did not have good outcomes. I imagine they’d have a much different point of view.”
Because doctors are treating babies before they show symptoms, and there’s some uncertainty about the kinds of genetic changes that cause the disease, it’s possible that some babies could be treated when they might not need to be, said H. Gilbert Welch, MD, a professor of medicine at the Dartmouth Institute in Lebanon, NH.
Parents bet on improved treatments
Kurtzberg and her team are now trying a new protocol, one that involves transfusing two sets of cells to try to improve outcomes for these babies.
Three-month-old Tygh DeRossett is trying that therapy. He was born Nov. 29, 2016, in Kentucky, a state that began screening babies for Krabbe disease last year.
When Tygh went for his first checkup, his parents got the awful news that he had screened positive.
Referred to Duke, Tygh began preparations for a stem cell transplant at 8 days old. He got a second set of cells when he was 28 days old.
“He’s pretty much excelled through everything,” says his mother, Amanda DeRossett. “There’s no sign of the disease.”
They were supposed to leave the hospital this week, but Tygh’s oxygen level keeps dropping at night. His doctors aren’t sure why.
Amanda believes Tygh will grow up to be a normal kid.
Asked how she feels about screening, now that they’ve been through the procedure, Amanda says, “I think the parents should at least be informed and have the option of doing the blood test.”
She adds, “I think it’s something that should at least be talked about.”
Correction:
An earlier version of this article incorrectly stated that an 18-year-old child who died last year was the oldest known Krabbe disease survivor. The oldest known survivor from the Duke program is now 22, according to Dr. Kurtzberg.
In addition to New York, three other states—Missouri, Kentucky and Ohio, have added Krabbe disease to their Newborn screening panels.
Six other states — Illinois, Louisiana, New Jersey, New Mexico, Pennsylvania and Tennessee — have passed laws that would allow screening but have not yet implemented their programs. In some of those cases, state health departments have blocked screening for Krabbe, citing both the expense of the testing and the lack of clear benefit from the treatment.
Brenda Goodman is a staff writer for WebMD. Her work has appeared in The New York Times, Scientific American, Psychology Today, The Boston Globe, Self, Shape, Parade, U.S. News and World Report, and Atlanta Magazine. She has a master’s degree in science and environmental reporting from New York University.
SOURCES:
April Garcia, Jackson’s mom, Lawrenceville, GA.
Brooke Adams, cousin of Cove Ellis, Cleveland, GA.
Lee Hawkins, Republican state representative, Gainesville, GA.
John Lantos, MD, director, pediatric bioethics, University of Missouri-Kansas City School of Medicine.
William Wilcox, MD, PhD, professor of human genetics, Emory University School of Medicine, Atlanta.
Joanne Kurtzberg, MD, director, pediatric bone marrow transplant program, Duke Children’s Hospital & Health Center, Durham, NC.
Roberta Salveson, PhD, clinical assistant professor, University of Washington, Seattle.
Anna Grantham, spokeswoman, Hunter’s Hope, Orchard Park, NY.
Melissa Wasserstein, MD, chief, division of pediatric genetic medicine, Children’s Hospital at Montefiore, Bronx, NY.
Amanda DeRossett, mother of a child with Krabbe, Puryear, TN.
New England Journal of Medicine, May 19, 2005.
Genetics in Medicine, December 2016.
Genetics in Medicine, June 2009.