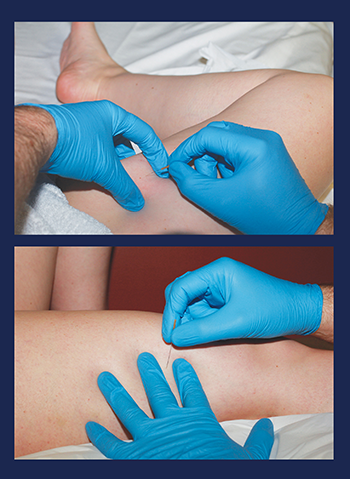
Troy Tribble, 41, turned to “dry needling’’ to ease his back pain and spasms.
He’s had several sessions. Each time his physical therapist works on a different area.
For Tribble, of Suwanee, it has made a world of difference.
The change he has experienced is “in my pain level and how frequently the spasms come,” Tribble says. It has helped him regain the quality of life that he used to have, he says.
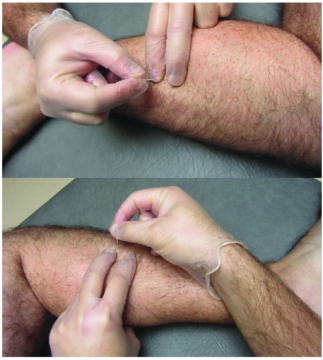
“If you don’t mind a little needle pricking,” it’s a worthwhile treatment, he says. “Compared to the pain that I was in, [the needle prick] didn’t matter.”
Dry needling uses a very fine (filiform) needle designed to go into sensitive muscle spots to relieve pain and improve muscle efficiency.
The needle is sometimes described as being thinner than the diameter of a cat’s whisker.
The dry needling procedure does not (and cannot) inject medication, as the needle has no opening for that purpose — hence, the word dry. It’s typically done by trained physical therapists.
Dry needling and acupuncture both use the filiform needle, but otherwise are considerably different.
With acupuncture, a healing technique developed more than 2,000 years ago in China, needles are placed into precise points along specific pathways called “meridians” and are left there for a period of time during the treatment.
With dry needling, a patient will point to a painful area. The physical therapist will insert a needle, then remove it (without the needle retention used in acupuncture). The purpose of each insertion is to reach a “trigger point,” causing a muscle to twitch.
As a way of treating pain, needling has attracted growing interest in the United States (and some other countries) over the last 20 years.
According to the American Physical Therapy Association (APTA), the performance of modern dry needling by physical therapists is based on neuroanatomy (the nervous system) and modern scientific study of the nervous and musculoskeletal systems (how muscles and bones work together).
Releasing beneficial chemicals
Needling achieves pain relief through the release of endorphins and serum cortisol and creates a balance in the body’s energy levels, says The Dry Needling Institute.
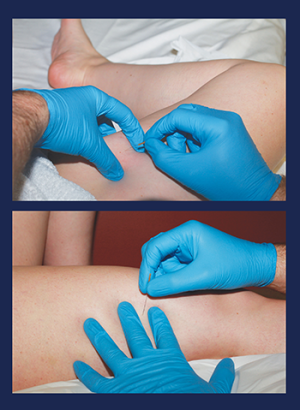
The institute says placing needles in the muscle’s trigger points results in “localized hemorrhaging, which promotes healing by stimulating collagen and protein formation.”
“The initial spasm that it creates feels very weird,” says Tribble, “but it goes away just as fast as it comes on.” It feels as if you have gone to the gym and worked muscle groups that you aren’t used to working, he says.
Nehama Schondorf, a physical therapist with Emory Rehabilitation Outpatient Center in Dunwoody, says dry needling can relieve local or “referred” muscular pain, improve range of motion and help improve strength.
Patients are willing to try needling if they can regain their range of motion in a joint — at least to some degree if not completely.
Schondorf says she recalls one patient with a ‘‘frozen’’ shoulder. The patient had tried everything from steroid injections to regular physical therapy with no relief. For her, the two or three sessions with needling led to real improvement.
“She was amazed by the change,” said Schondorf. For patients who have been helped by needling, the relief from pain is priceless.
Joseph Donnelly, president of the Physical Therapy Association of Georgia, says “If you have a myofascial trigger point within a muscle that feels like a knot, or there is a taut area in the muscle — it hurts.”
Donnelly serves as clinical associate professor at Mercer University’s Atlanta campus.
“The part that hurts the patient is actually a contracture,” says Donnelly. “Patients point to where it hurts. Of course, the names they use to describe the pain are varied, based on their discomfort. Myofascial pain is likely not one of them. “

The patient can usually steer the PT to a sore spot. Then, Donnelly explains, the PT allows the filiform needle to penetrate the trigger point (within the muscle) to get the desired twitch response.
This response can decrease pain that is generated from the muscle, improve muscle efficiency and decrease compressive loading across the involved joint — especially if the patient has experienced some degeneration.
There have been some professional turf battles between advocates of acupuncture and supporters of dry needling. This kind of rivalry is unfortunate, Donnelly says. The two kinds of treatment “are both good, and each has its place.”
What Donnelly proposes is that acupuncturists and physical therapists consider what is best for the patient’s condition.
“Just make patient care first,” he says.
Elaine Jones, a physical therapist at OrthoAtlanta in Newnan, agrees. The patient is paramount, she says.
Jones points to many examples of patients who have found relief when a trigger point dry needling procedure was included in their treatment plan.
Quite common is the patient who may experience severe neck strain and headaches, resulting from unusually prolonged periods of precise, focused and stressful work ending in an overuse injury. Jones says, “Patients have realized relief after enduring post-operative foot pain.”
Side effects
Physiatrists — physicians trained in physical medicine and rehabilitation — focus on non-surgical methods to restore optimal function. They are licensed to administer “trigger point injections,” a category that incorporates injecting medication as well as needling.
“Dry needling can be painful,” says Dr. Michael McHenry, a physiatrist at OrthoAtlanta. “Physiatrists can use medications to make the needling process less painful, and other medications that can provide relief over a longer duration,” says McHenry.
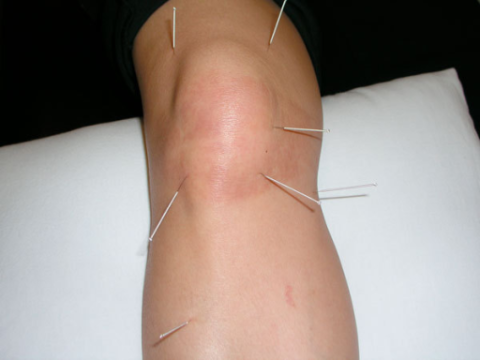
In fact, the physiatrist may incorporate dry needling into a larger treatment plan for the patient being served by the physical therapy team.
“It is not a positive fix,” said Donnelly when referring to the technique. “Patients need to engage in the therapeutic process, too.” That means staying true to their recommended home exercise program, especially when it comes to retraining for posture.
Dry needling can be used as part of complex treatment for chronic musculoskeletal pain and can be applied by physiatrists, family physicians, rheumatologists, orthopedic surgeons, pain specialists, dentists and physical therapists, according to the APTA.
Each state mandates what is allowed within a health professional’s scope of practice. When it comes to dry needling, states’ rules vary widely.
In Georgia, an otherwise qualified professional requires an additional 50 hours of training to perform needling therapy.
Boards in five states — Idaho, Kansas, Idaho, New York and South Dakota — have stated that needling is not within the scope of practice. And the Hawaii physical therapy statute contains language prohibiting physical therapists from puncturing the skin for any purpose.
Judi Kanne, a registered nurse and freelance writer, combines her nursing and journalism backgrounds to write about public health. She lives in Atlanta.