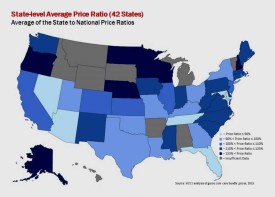
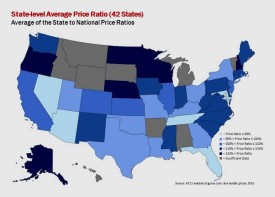
A new study shows a wide variation in health care prices between states – and often between cities in the same state.
The study, published Wednesday in the journal Health Affairs, found that Georgia health care prices for the privately insured are below the national average.
Some states, meanwhile, pay more than double what other states pay, according to the study from the Health Care Cost Institute.

The HCCI uses commercial insurance to chart differences in prices for more than 240 common medical services. The prices studied are total payments received by a medical provider – both from the insurer and the consumer, which includes co-pays and co-insurance.
Compared to the national average, Alaska has the highest average health care prices, followed by Wisconsin, North Dakota, New Hampshire and Minnesota. In Arizona, Florida, Maryland and Tennessee, more than 90 percent of health care services are priced lower than the national average.
Health care has seen an increasing push toward more transparency in pricing, and insurers as well as other organizations have brought more data into the public realm.
“Consumers are entitled to this information,” David Newman, executive director of HCCI, told Georgia Health News on Wednesday.
The data, derived from 1.8 billion claims, are for the years 2012 and 2013, but the prices were updated to more current estimates by applying trend factors, the report said.
The state variations in prices are reflected in knee replacements in California, with a $27,243 average price difference between Riverside ($30,261) and Sacramento ($57,504). In Ohio, the average price of a pregnancy ultrasound in Cleveland was almost three times that in Canton ($522 and $183, respectively), even though the two cities are only 60 miles apart.
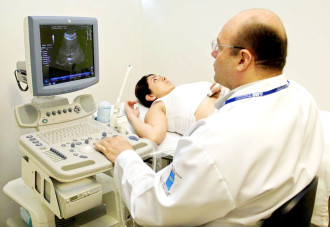
Newman said that in Georgia, the average price for a pregnancy ultrasound is $337. Atlanta’s price averages $338, but in Macon, the price is $411, and in Athens, it’s $247.
Meanwhile, allergy testing is more expensive in Georgia than the U.S. average — $1,823 vs. $1,220. Macon’s average price is $2,316, while Savannah’s is $1,412, Newman said.
Other services where Georgia prices are above the national average include administration of flu vaccine for adults; shingles vaccination; radiation treatment; testing for mononucleosis, strep throat and tuberculosis; urinalysis; and a bone density study.
The Georgia prices don’t include those of Blue Cross and Blue Shield of Georgia, the state’s largest insurer, which Newman said declined to participate.
The study does not pinpoint causes of the price differences.
Newman said the goal is to have employers, insurers, and leaders of government health programs look at the variations and ask why some procedures are priced higher than average.
“It’s our hope,’’ he said, “that where there’s price transparency, providers have a stronger tendency to lower prices.”
Prices vary more for some health care services than for others. For example, states have similar prices for acupuncture, while prices for cataract removal vary significantly from state to state, the study’s authors said. The greatest variation in prices was observed for imaging, radiology and lab tests.
Newnan said that in some cases, higher prices may actually help ease a situation where there is a shortage of medical providers delivering a service. Those high prices, he said, may attract other providers to that area.
Bill Custer, a health insurance expert at Georgia State University, pointed out that the study did not factor in cost of living in the individual states. Custer noted that California and Georgia have relatively the same level of pricing as compared to the national average, but that in California, “the cost of living is much higher.’’
And the data don’t include the medical outcomes of the services. “If the cost is higher, are you getting desirable outcomes?” Custer said.
Georgia has some wide variation in pricing, he said.
But there are some limits to health care price comparisons, Custer said, adding that often consumers who are in “narrow’’ insurance networks don’t have as much choice as to where they obtain a particular medical service.
Nine states were omitted from the study. Eight of them — Alabama, Hawaii, Idaho, Michigan, Montana, South Dakota, Vermont and Wyoming — were left out due to insufficiency of data or because of state statutes that discourage data sharing, the authors said. Arkansas was omitted because it signaled that it did not want its state data compared to national data, HCCI said.