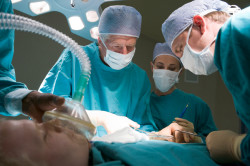
What’s the price tag of a leg amputated as a result of a doctor’s negligence in the operating room?
It can easily be $3 million in the United States. In my native Germany, it may be $30,000.
That’s a catchy and somewhat unfair comparison, of course. But it points to a highly controversial subject: medical malpractice reform.
A recent proposal to fix the broken tort system came in Georgia’s Patient Compensation Act, or Senate Bill 86.
Introduced by Sen. Brandon Beach (R-Alpharetta), the bill would have created an administrative system to handle patients’ claims outside the courts. Patients would not need lawyers to propel their cases forward; health care practitioners would have to pay into an administrative fund instead of purchasing costly malpractice insurance; and payments to patients would be made within months rather than years.
SB 86 was introduced in the Georgia Legislature in February. It was hailed by physicians, attacked by trial lawyers, and never passed out of the Senate Health and Human Services Committee.
But SB 86 could make a comeback in next year’s General Assembly, as other proposals for tort reform are springing up around the country.
A broken system
Many health care experts say the U.S. tort system is costly, unreliable, ineffective and counterproductive – in short, broken. Even though the number of claims has declined, medical litigation costs in America are still more than twice as high as in other developed countries, such as Canada, England and Germany.
According to a RAND study from 2011, 99 percent of physicians in high-risk specialties, such as neurosurgery and obstetrics, face at least one malpractice claim during their careers. For their colleagues in Europe, there’s only a roughly 20 percent chance of a lawsuit.
The premium for medical liability insurance for a general surgeon in the United States can be as high as $130,000 to $190,000 in areas such as Long Island, N.Y., or Miami. In Germany, it’s between $5,000 and $10,000.
The main reason for the dire state of the U.S. medical malpractice landscape seems to be that the system offers patients too many incentives to sue doctors for bad outcomes (and sometimes for overall bad luck in life) rather than for bad treatment.
While there’s no medical malpractice nirvana, and foreign liability models may not fully translate into the American system, looking beyond U.S. borders may still offer some insights and, possibly, inspiration.
Take, for example, the fact that in Canada, Japan and most European countries, judges, not juries, try medical litigation cases. One benefit of such systems is that they increase reliability and consistency in rulings.
Keeping the jury out of the courtroom also helps soften the adversarial, high-drama litigation style that’s common in jury trials, and helps keep extreme claims and awards in check. In Germany, standardized reimbursement tables for economic and non-economic losses guide the judges’ rulings.
A cap on damages
Also, in many European countries, mediation and arbitration are mandatory before a case can proceed to court, and that has yielded high success rates. While denying patients the right to be heard by a jury of their peers may raise constitutional concerns in this country, voluntary mediation does not.
Another common way to manage medical malpractice lawsuits – not only abroad, but in some U.S. states as well – is putting a cap on damages. In the United Kingdom, the amount awarded for pain and suffering is usually capped at about $400,000, though exceptions apply. In Germany, a pain-and-suffering-award of $500,000 is considered high and applies only to the most severe cases of medical malpractice, such as those that result in birth defects.
But comparing awards in Europe and America can be misleading. In many European countries, social safety nets and welfare systems provide additional coverage for victims of medical malpractice. In Germany, disability costs resulting from a treatment error are for the most part covered by the social security system. In the U.S., damage caps would not only put poorer and elderly patients at a disadvantage, they would also discourage lawyers from taking on a medical malpractice case.
This brings me to the next point: lawyers’ compensation.
In Canada and most European countries, contingency fees for lawyers are generally prohibited. In the United States, these fees are often 30 percent to 40 percent of the final award. They create a huge incentive to file a lawsuit and are seen by some physicians’ lobbyists as a “parasitic form of venture capitalism.”
In Germany, the loser often has to pay the other side’s legal costs – a rule that’s been heavily criticized by consumer advocates who argue that it puts low-income patients at a disadvantage. But many Germans have legal expense insurance, which covers policyholders against the potential costs of legal action. Low-income citizens who can’t afford such insurance may be eligible for government-subsidized legal aid.
The culture of doctors
Finally, different medical malpractice cultures create different types of doctors. Different cultures affect doctors’ behavior, and shape the doctor-patient relationship differently. Neither result may be desirable in the end. In the United States, many doctors feel pushed to practice “defensive medicine,” doing unnecessary tests on patients just to shield themselves from the accusation that they did too little. This phenomenon is starting to take hold in Europe as well. Still, American physicians today order 70 percent more CT scans per capita than their colleagues in Germany.
Also, many physicians in the United States report that they often feel pressured to settle cases that might be defensible in court, and hence they are manipulated into admitting to errors they didn’t make. If the doctors don’t settle, they fear that plaintiffs might try to destroy their reputations in online forums or by other means.
In most of Europe, parties engaged in a lawsuit are advised by their lawyers to refrain from publicly commenting on a pending case or on the other parties involved. Also, most European countries have tighter defamation-of-character and reputational-damage laws than America, where the right to freedom of speech would render most “gag orders” unconstitutional.
It’s probably true that doctors are protected in most industrialized countries more than they are in the United States – legally, ethically and socially.
But there’s a flip side, as seen in my native Germany. There, for many historical and cultural reasons, physicians still enjoy a reputation of being what Germans sarcastically call “demigods in white” – meaning they consider themselves as authorities not really to be questioned, more or less untouchable by law, defamation or any other pressure.
It seems that either system, in the end, somehow backfires on the patient. In America, it may be physicians who put up their guard and prefer to play it safe, having decided not to trust their instincts on what patients need. In Germany, it can be doctors who often consider themselves and their decisions above the law and treat patients with an air of arrogance and immunity.
With many best and worst practice examples under consideration, and the call for medical malpractice reform in the United States getting louder, Georgia’s Senate Bill 86 seems, after all, to deserve a second look – maybe even as a blueprint for a wider solution.
Katja Ridderbusch is an Atlanta-based foreign correspondent for German news media, including the national dailies “Die Welt” and “Der Tagesspiegel,” as well as German national public radio. She frequently reports about health care in the United States.