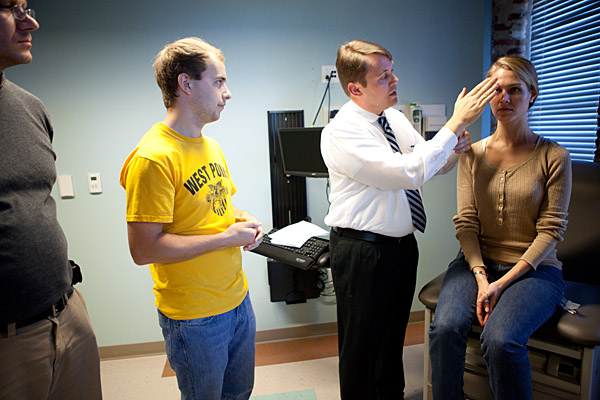
When most people visit the doctor, they are probably not thinking of anything but getting individual care. But it’s becoming more common for providers to look past individual blood glucose levels and cholesterol counts to the social factors that affect the health of whole communities.
That’s why the GHSU/UGA Medical Partnership and the UGA College of Public Health have joined forces to create a new option for medical students who want to earn a master of public health degree along with their medical degree.
“Doctors in the future are going to be responsible for care outside of the office,” said Dr. Stephen Goggans, an internist who teaches Partnership medical students while working toward an MPH degree of his own. “They’ll be responsible for intervening in the environment and for thinking about the health of whole groups of people.”
Dual-degree programs aren’t new at UGA. The schools of veterinary medicine and social work already offer degrees in conjunction with the master of public health. When the MD/MPH program is officially approved at UGA – and possibly enroll students in 2012 — it will become the third in Georgia, joining programs offered at Emory and Morehouse.
Georgia appears to be part of a national trend, according to the Association of American Medical Colleges. At least 75 U.S. medical schools now make public health education available to future doctors.
Public health and medicine have sometimes seemed to be totally distinct fields: Doctors and other providers focused on treating illness, one patient at a time, while public health officials were concerned with the health of entire populations. But now the lines are blurring.
“Medical education has historically not been very committed to teaching about the health of populations or even measuring outcomes beyond one patient at a time,” said Dr. Richard Schuster, a member of the committee designing the program and a professor at the UGA College of Public Health. “When you’re not feeling well, you certainly want to be taken care of as an individual, yet modern medicine requires an understanding of systems and how patients fit into communities.”
An accent on prevention
[youtube]http://www.youtube.com/watch?v=rmb-bTiWqFE[/youtube]Given that health is strongly influenced by factors such as poverty, lack of education and unemployment, a public health approach to medicine will inevitably focus more attention on such issues. For Georgia, where physicians are in short supply and access to health care is uneven, doctors with an eye for public health can make a big difference. They may incorporate more preventive advice into primary care visits or seek leadership positions so they can change policy.
Thinking of patients as parts of a larger community means shifting the focus of medicine to prevention, whether the issue is lowering risk for chronic diseases like diabetes and heart disease, or carrying out classic public health functions such as immunization and health education.
At most medical schools that have dual degrees, 5 percent to 10 percent of students pursue an MPH along with their MD, according to Dr. Cheryl Dickson, associate dean for student and multicultural affairs at the GHSU/UGA Partnership. She anticipates this will be the case at the Athens campus, where med students are already expressing interest.
Russell Ledford is one of those students drawn to the meshing of public health and medical education.
“I can see myself doing more ‘forest and not the trees’ kinds of things down the road,” said Ledford, a first-year student at the Partnership. “But I am also really attracted to . . . individual care and building relationships with people.”
Students who pursue both degrees often end up in positions that give them the ability to change health policy – whether they’re employed in a county health department, serving as chief medical officer at a hospital, or working at a federal agency. In Georgia, many district health directors – who oversee public health programs in multiple counties – are MD/MPHs.
“You want to attract students who want to go beyond the care of the patient on a one-by-one basis,” said Schuster, who has helped create similar programs at other institutions. “They intuitively know they need something more, and they see the world very differently.”
Medical students who want to earn an MPH at UGA will be able to take public health classes concurrently with their medical coursework, or they can step out of the med school curriculum for one year and complete all of their MPH courses at an accelerated pace. Either way, they should be able to finish both degrees within five years.
Graduates of such programs are prepared to see both the clinical and social sides of health.
“You make people who are really unique in that they are thinking simultaneously about public health and the individual care of a patient on a moment-by-moment basis,” said Schuster.
Going beyond the merely medical
The UGA College of Public Health requires its students to take classes in five core areas: epidemiology, biostatistics, environmental health, health promotion and behavior, and health policy and management. Dual-degree students will study everything from health care finance and grant writing to the social determinants of health and developing health programs, and they will gain real-world experience through a public health-related project in the community.
“They’ll have this unique population health perspective that you don’t necessarily have at the end of medical school,” said Dr. Laurel Murrow, a clinical educator at the med school who is also on the program design committee. “And they’ll have concrete skills in an area they choose.”
Dickson believes that doctors with public health training are more attuned to patterns in their communities, such as elevated rates of diabetes or obesity.
Ledford plans to go into primary care in a rural area where he can use his MPH to focus on community planning and prevention for those types of diseases.
“It never gets old trying to help people stop smoking, to help people diet correctly, and I think those things will continue to be an issue,” said Ledford.
“When you focus on bigger groups, you can’t help but be drawn to disparities,” said Goggans. “When medicine as a whole starts thinking about this, the biggest beneficiaries are going to be those groups, because that’s where the real chances for improvement are.”
Goggans says what he’s learned in public health courses helps him teach health policy sessions for second-year medical students. In the future, he hopes to collaborate with the public health researchers who are now his teachers.
Faculty members from both the medical school and the College of Public Health see the dual-degree option as an added benefit – for students, the university, the surrounding community and the state.
“It’s the right thing to do,” said Schuster. “They [MD/MPH students] are, to put it simply and with some bias, the future leaders of medicine.”